Unless the state’s plan to curb maternal deaths is wholly implemented, it won’t make a dent.
Also written by Natasha Rhoda & Bob Pattinson
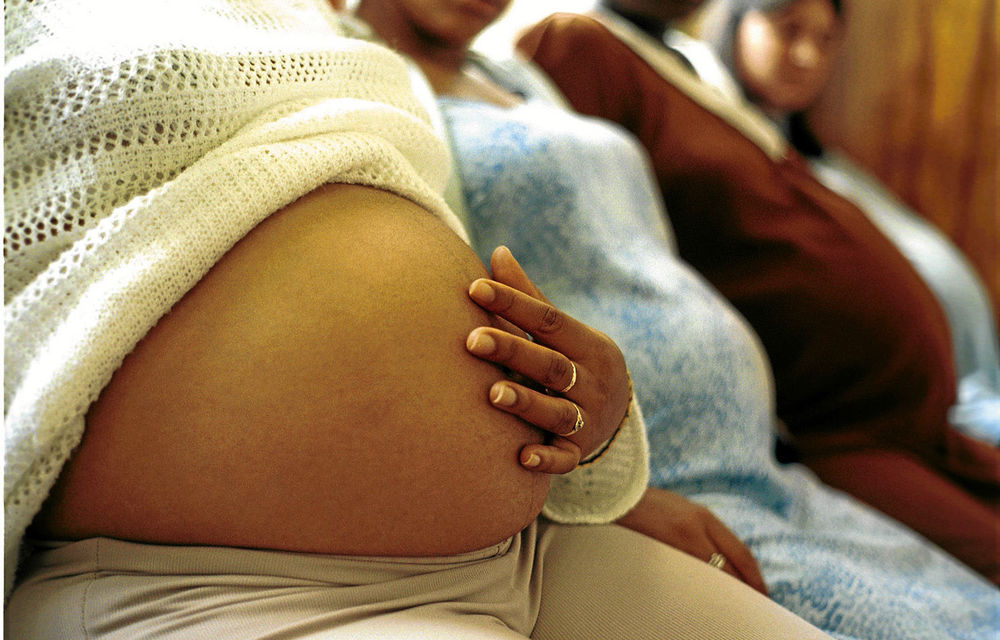
A Bhekisisa article, “When mother is snatched away, Gogo picks up the pieces” (Mail & Guardian, July 12), highlighted South Africa’s unacceptably high maternal death rate.
It also focused on the appalling consequences for families and society as a result of mothers’ deaths: “South Africa’s maternal mortality rate leaves the elderly to deal with its consequences, with many unable to keep up,” the article said.
There is a high level of ministerial political will and instruction to officials to tackle this problem with vigour and determination.
The latest available government estimates are that 260 out of every 100 000 South African women die during pregnancy or labour, or within 42 days after giving birth.
Early indications from 2011 and 2012 government data show that the number of maternal deaths due to HIV are being reduced and, consequently, the total number of deaths is also on the decline.
However, as indicated in the article, there are many aspects of maternal health services that need improving. Slowly but surely these are being addressed.
The Free State is an example of how quickly things can improve. Between 2011 and 2012, maternal deaths fell from 122 to 76 – a 48% reduction in a year. This improvement has continued throughout 2013.
The decrease in mortality was due to a number of interventions – one being a significant reduction in the time it took to transfer critically ill pregnant women between healthcare facilities through improved use of emergency medical services (ambulances).
The centralisation of facilities where caesarean sections can be carried out and ensuring that these are fully staffed 24 hours a day also contributed to the reduction in women who died.
Lastly, getting all health workers involved and better use of data to monitor what is happening with maternity services all had a positive effect on maternal mortality figures.
However, despite this progress, South Africa is still far behind on meeting the United Nation’s millennium development goal to improve maternal mortality figures to 38 deaths per 100000 in 2015 – the country’s figure of 260 deaths per 100 000 is still higher and there are only 850 days left to achieve this target.
Unless there is a robust programme to deal with HIV and the other causes of maternal and child mortality in South Africa, we will fall short of meeting the targets.
A recent study by researchers from the London School of Hygiene and Tropical Medicine found that in countries with a high HIV prevalence, such as South Africa, one in four pregnancy-related deaths is due to HIV. This backdrop of HIV and its associated problems increases the number of deaths of pregnant women, infants and children under five.
There are also problems related to the quality of care that pregnant women, infants and young children receive.
To address this, three ministerial committees have been established to look at maternal, neonatal and children’s deaths and the associated avoidable causes.
These committees comprise local experts and their annual reports provide the evidence for policy-making in the ministry of health.
When Minister of Health Aaron Motsoaledi came into office in 2009 he signed a performance agreement – the negotiated service delivery agreement – in which he, as well as the nine provincial MECs for health, committed the sector to contribute to the government’s vision of “a long and healthy life for all South Africans”.
Two of the four goals are “to increase life expectancy “and “decrease maternal and child mortality”.
Parallel to this internal commitment to improve maternal and child health there is also an external commitment in the form of the campaign to accelerate reduction of maternal, neonatal and child mortality in Africa.
This campaign was launched during the African Union Conference of Ministers of Health in May 2009 in Ethiopia.
In May 2012, South Africa launched its own campaign to accelerate reduction of maternal, neonatal and child mortality. It has various goals:
Access to contraception
A new contraceptive policy will be launched later this year. It will increase the range of contraceptives available in the public sector as well as increase the knowledge, skills and attitudes of front-line health workers who provide these contraceptives.
Early access to services
In the public sector, many pregnant women have not been attending antenatal clinics early in their pregnancy.
The earlier a pregnant woman attends the more likely she is to get optimal benefit from the services available.
Access to skilled personnel
Deliveries will be handled by maternity waiting homes and dedicated obstetric ambulances will be provided.
Medical skills
Doctors and midwives will be trained in essential steps in managing obstetric emergencies.
This will increase knowledge and skills of healthcare providers in managing obstetric emergencies.
So far, more than 2 000 doctors and nurses have been trained and by the end of 2014 all maternity units in the public sector will have a doctor and midwife trained in the management of obstetric emergencies.
Health of premature babies
Lactating mothers’ facilities will be established and “kangaroo mother care”, where mothers keep their babies warm by swaddling them skin to skin on their chests, will be strengthened.
Good baby feeding practices
Exclusive breastfeeding will be promoted – that is breast milk only for the first six months of the babies’ life.
Transmission of HIV
All pregnant women will be tested for HIV – private doctors would be required to do so too. This will identify those who are HIV infected and will enable these mothers and their babies to get antiretroviral drugs.
This will help the health of the mothers and also prevent HIV infection of the baby before or during birth, or while breastfeeding. The proportion of babies at risk of HIV infection who are infected with HIV at six weeks of age has dropped, from 9.6% in 2008 to 2.4% in 2012.
Early results from the ministerial committee dealing with maternal deaths show that there were 250 fewer maternal deaths in 2011 from HIV-related causes than in 2010.
Immunisation coverage
In recognition of the fact that diarrhoea and pneumonia are two of the biggest killers of young children, two new vaccines, rotavirus for diarrhoea and pneumococcal conjugate vaccine for pneumonia, were introduced into the immunisation schedule for infants in 2009.
Since then, more than 90% of eligible children have received these vaccines.
As a result, the number of cases of diarrhoea has fallen from 14 per 100 children a year in 2009 to 10 per 100 children in 2011. It has been estimated that the introduction of these vaccines has reduced child mortality by at least five deaths per 1 000 births.
Recognising that the effective implementation of the interventions listed above is dependent on front-line workers performing their duties with good attitudes and having the appropriate skills, district clinical specialist teams were introduced into all 52 districts in 2012.
Each specialist team consists of doctors and nurses who have specialised training in an area relevant to maternal and child health. Their job is to improve the quality of care throughout South Africa so that there are fewer maternal, infant and child deaths, and improved health for mothers and their babies.
The national health department is confident that these teams and the interventions described above will get South Africa back on track to achieving the millennium development goals.
Recent results from the Medical Research Council show that there has been a dramatic improvement in under-five and infant mortality, with a 25% reduction over a two-year period.
Neonatal mortality, which is the deaths of newborn babies in the first four weeks of life, has not fallen for the period 2009-2011.
There are, however, cost-effective and proven neonatal interventions such as kangaroo mother care, exclusive breastfeeding, strict infection control and respiratory support for preterm babies, which when implemented together can reduce neonatal mortality.
It is these neonatal interventions that the newly appointed specialist teams will focus on and oversee implementation of at the district level, in a bid to reduce neonatal deaths.
Peter Barron is a public health specialist and technical assistant at the health department. Neil McKerrow is a paediatrician and the chair of the department’s national child morta-lity committee. Jack Moodley is an obstetrician and chairs the ministerial committee on confidential enquiries into maternal deaths. Natasha Rhoda is a paediatrician and a member of the national perinatal and neonatal morbidity and mortality committee. Robert Pattinson is an obstetrician from the University of Pretoria and a member of the ministerial committee on confidential enquiries into maternal deaths