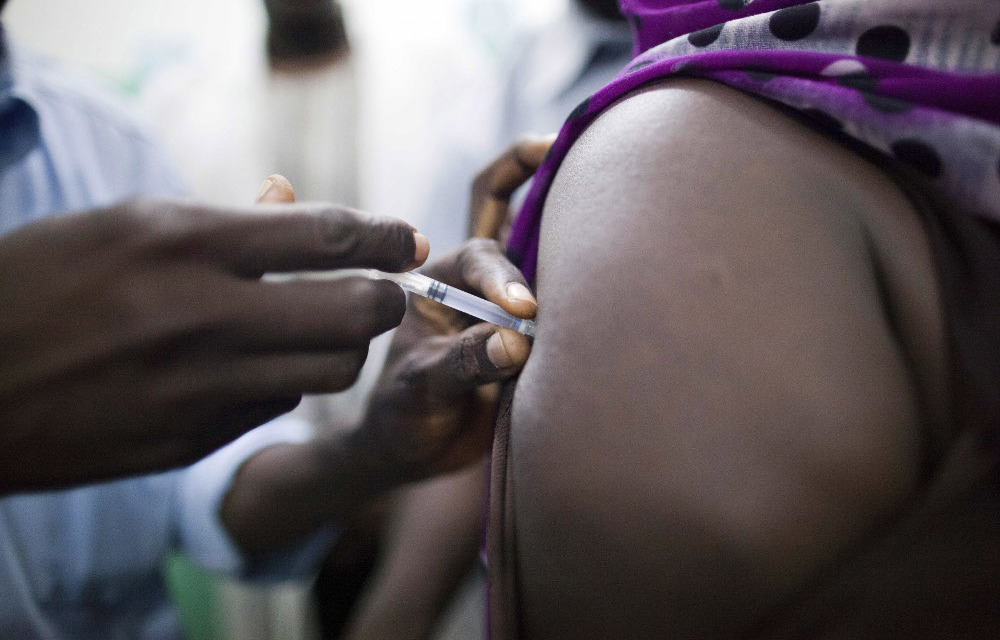
Only six out of ten Angolan children have been vaccinated against yellow fever.
Angola is currently experiencing the biggest yellow fever outbreak the country has seen in 30 years. According to the World Health Organisation (WHO), the outbreak, which has its epicentre in the capital, Luanda, has affected 16 of the country’s 18 provinces. The health body says there have already been hundreds of cases and 178 confirmed deaths from yellow fever in the country.
The yellow fever virus is transmitted by Aedes or Haemagogus mosquitoes and causes fever, pain, nausea and vomiting. At its most severe, there can be bleeding, jaundice and organ damage. The United States Centres for Disease Control and Prevention says up to half of those who are severely affected by yellow fever will die.
A single yellow fever immunisation, which Angola’s vaccination schedule recommends all babies receive at nine months, provides lifelong immunity to the disease.
But according to the Angolan health ministry’s multi-year immunisation plan for 2011 to 2015, rates of yellow fever vaccination dropped from 72% in 2007 to 40% in 2009 and 2010, owing to vaccine stock-outs. By 2014, this had increased to 64%, according to the WHO.
WHO spokesperson Dr Margaret Harris says the organisation has mobilised vaccines from the yellow fever vaccine stockpiles set up ten years ago to ensure the WHO can get vaccines to a population rapidly if an outbreak like this one occurs.
According to the vaccine initiative, Gavi, emergency yellow fever vaccines are stockpiled at sites in Senegal, France and Brazil and countries can request access to these during outbreaks.
The yellow fever vaccine, which has been available since the 1930s, is almost 100% effective. The WHO recommends the vaccine for everyone older than nine months who live in yellow fever endemic areas, as well as for people travelling to areas where yellow fever is a risk. In the past, a booster vaccine was needed after 10 years, but in 2013 the WHO revised its recommendations, saying the booster is no longer required.
Harris says that vaccination programmes have reduced yellow fever outbreaks in many countries in recent years.
“Where vaccination rates are high, yellow fever is much less of a problem. In West Africa, where outbreaks like this used to be a yearly occurrence, mass yellow fever vaccination campaigns have made yellow fever outbreaks rare,” she says.
According to the WHO, since yellow fever vaccination began in the 1930s, “only 12 known cases of yellow fever post-vaccination have been identified, after 600 million doses have been dispensed”.
But Harris says routine childhood vaccination, which includes the yellow fever vaccination, is not reaching nearly enough children.
In Angola only six out of ten children received the vaccine in 2014, according to health ministry data.
The WHO is working with its partners and the Angolan government to vaccinate those at risk. An immunisation programme launched in the Viana district of Luanda province in February initially targeted 1.5-million people. Harris says the WHO is negotiating with the world’s four yellow fever vaccine manufacturers to make more vaccine available quickly.
The biggest challenge at this point is getting enough vaccine to Angola quickly enough to vaccinate everyone at risk, she says.
“To do this we have to buy more vaccine and spend operational money – transport, support systems, vaccinators, etc – which we estimate will cost at least $3-million. Another important thing is if people are exporting yellow fever to other countries this suggests they have not been vaccinated: it is really important that anyone travelling to a yellow fever endemic country gets immunised against yellow fever,” she says.
Harris says that while most of the yellow fever have been in Luanda, some cases were exported by people travelling back to their home countries in the Democratic Republic of Congo, China (Beijing) and Kenya. Namibia and Zambia are also on high alert for imported cases.
Another factor driving the spread of the disease is urbanisation. The WHO has in the past warned that “large and uncontrollable outbreaks” in urban areas are more likely than ever due to rapid urbanisation, which has resulted in large populations of people living in high density areas, where there are also large populations of the organisms that spread disease in this case mosquitos. According to the health body, urban growth rates in Africa are almost twice the global average.
In addition to the vaccination programme, Angola has also embarked on a vector control programme. This involves stopping the mosquitoes that spread yellow fever from breeding where humans live, by scraping water containers and using larvicides to destroy the eggs, and by cleaning up rubbish sites, where mosquitoes are known to lay their eggs in tyres, plastic bags and other small containers that collect water. Health officials are also encouraging people to sleep under bed nets.
Faranaaz Parker is the former Bhekisisa news editor.