This country tested out a national health insurance. Find out what happened next.
Rajiv Gupta has a distinct spring in his step. He has brought his mother to New Delhi from the northern state of Bihar for a hip replacement, for which he won’t have to pay. His mother qualified for free treatment under Ayushman Bharat, the government’s ambitious new health insurance scheme.
“I can’t quite believe this is happening. When the doctors in Bihar told me it would cost 200 000 rupees (about R41 000), I took mum home. That kind of money is impossible for me. I just run a tiny sari shop. And now she’s getting it done here free,” says Gupta. Then he hurries off as though scared he has got it wrong and someone is going to present him with a bill.
Millions of people in India live in fear of getting sick, and not just because of the physical symptoms. For some, the cost of treatment can be equivalent to two years’ wages.
Launched just under six months ago, Ayushman Bharat aims to provide 500 million Indian families with health insurance of 500 000 rupees (about R102 645) a year for secondary and tertiary medical care. Those eligible are the most vulnerable sections of the population.
Rapid economic growth over two decades has improved the lives of millions of people, but medical care is still unaffordable for many. Though a doctor’s consultation in government hospitals is largely free, patients have to pay for implants or stents, along with medical consumables. The cost of hospital treatment can be catastrophic, pushing an already poor family into debt.
“It is early days, but this is a game-changer,” says Dr Randeep Guleria, pulmonologist and director of the All India Institute of Medical Sciences (AIIMS) in the Indian capital. “Hospital treatment is an impossible cost for the poor – even for sections of the middle class. It’s a godsend to those who would have been kept at home by their families and left to die.”
Finance minister Arun Jaitley said recently that 62% of the Indian population have to pay healthcare bills themselves and most find it unaffordable. On Wednesday he said it was fast becoming the world’s largest free healthcare scheme.

According to official data, more than 20.3-million Indians have so far qualified for the scheme. About 1.4-million people have received free treatment.
While the scheme is off to a good start, Guleria says challenges remain. The biggest is making people aware of it. Although almost 8-million people have checked on the Ayushman portal to see if they are eligible, some patients at Guleria’s hospital had no idea they could become part of the scheme.
Attempts are being made to inform the public, even in the remotest villages. Posters and banners are up at railway stations. When he drives to work, Guleria hears the radio station repeatedly playing a government jingle urging listeners to dial a number to check if they could benefit.
The national health authority, which runs the plan, is teaming up with Uber, Flipkart, Amazon and other companies to access their employee database. The scheme’s CEO, Indu Bhushan, believes many of their employees will be eligible and must be tracked down to be told of their rights.
“Currently, about 400 000 people are registering every month. We want to push this up to 1 million a month,” said Bhushan.
A second challenge is fraud, which Bhushan is anxious to prevent. “Abuse will not only be an extra financial burden, it will damage our reputation, so we need to clamp down firmly right away on fraud, on people falsely claiming this benefit, or on hospital and patient collusion to cheat the state,” he says.
A third issue is persuading more private hospitals to join the scheme. The free treatment is to be offered in government and independent hospitals, but the involvement of the latter is crucial.
Only a handful of government hospitals, such as AIIMS, offer specialist care for complex treatments and procedures, according to Girdhar J Gyani, director general of the Association of Healthcare Providers of India. “More than 80% of tertiary care in India is provided by private hospitals. But the reimbursement rates under Ayushman are irrational and far too low,” he says. “So, for example, the reimbursement for a knee replacement is nowhere near the cost incurred by a private hospital.”
If the scheme is to be implemented in letter and spirit, he added, the reimbursement rates have to be increased. The government has set up a committee to review the rates.
That said, about 6 000 private hospitals, mainly smaller ones, have joined the scheme. Some beneficiaries have been surprised to find themselves being treated at a private hospital, the exclusive enclave of the wealthy. About 60% of the scheme’s patients have been treated in private hospitals.
Shah Mohammed, 50, is recuperating at SGT hospital in Gurgaon, a large private institution in the middle of a deserted, dusty plain that caters to the surrounding villages. Mohammed suffered a fractured jaw and haematoma after his scooter crashed into another vehicle.
“I hadn’t heard of this Ayushman,” he says. “But when I was admitted here, the staff checked and found that I qualified. I can’t get over the fact that when I am discharged, I will walk out of a private hospital without paying a rupee.”
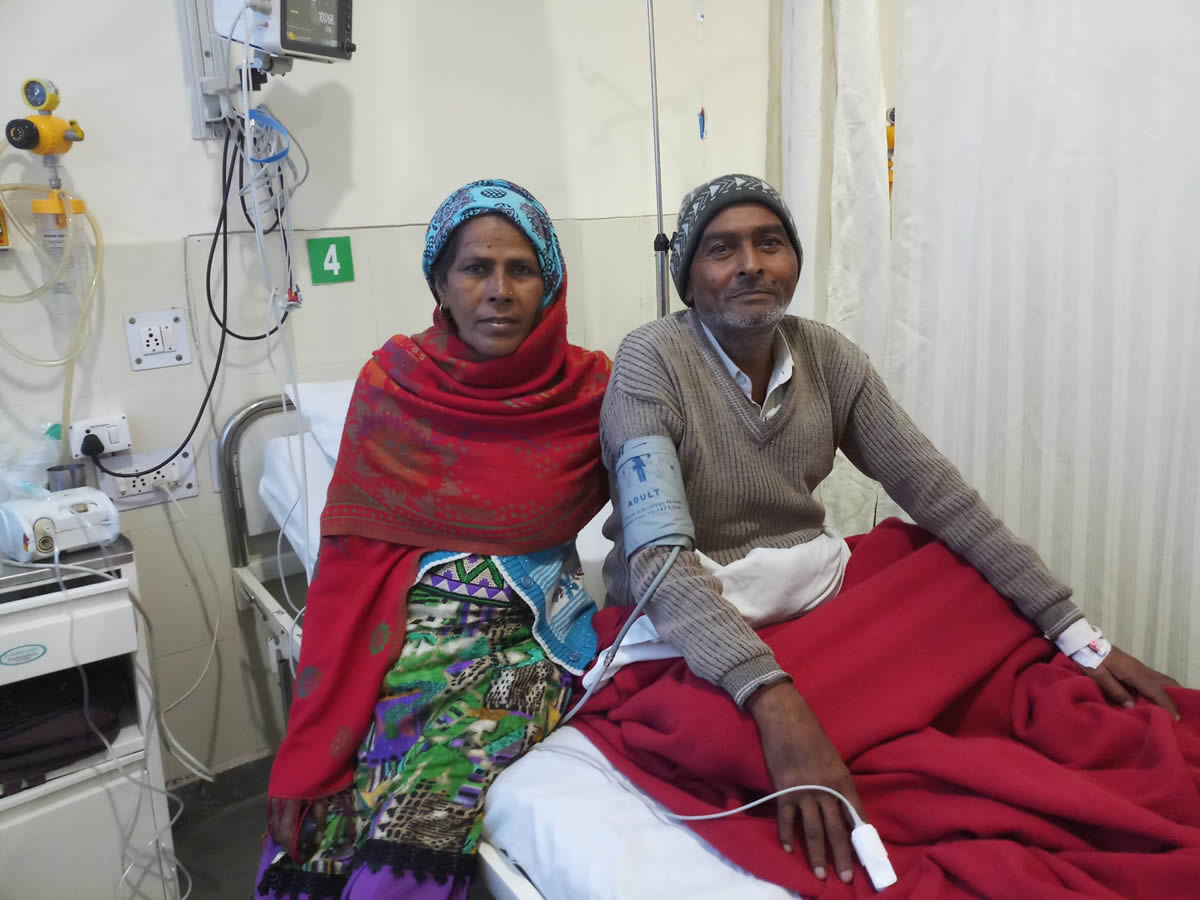
In another ward at SGT, Ramesh Kumar, a 50-year-old tailor, is recovering from respiratory failure. “My wife would have had to borrow money. We just don’t have that kind of cash at home. I knew it was going to be free but I didn’t expect to be treated at a private hospital,” he says.
Government or private, none of this matters to Sunny Kumar and his mother, Asha. Their father has been operated on for a hole in the heart at AIIMS and is doing well. “This is the first time the government has done something really concrete for the poor,” says Asha.
Nine-year-old Shiv Shankar Kumar suffers from a leaky heart valve. When his father, Mahesh Mandal, was told in his hometown of Bihar last month that treatment would cost 300,000 rupees, he took Shiv home. “My wife and I had no choice but to leave his fate to God,” says Mandal.
Later, he heard about Ayushman Bharat and registered. The day after he received his gold card, he picked his son up in his arms and boarded a train to AIIMS. Shiv has been successfully treated. Mandal swipes his phone to show his picture. “I can’t wait to take him home so that he can start his life again,” he says.
This is an edited version of a feature originally published as part of The Guardian’s Global Development project.
Amrit Dhillon is a freelance journalist based in New Delhi.



