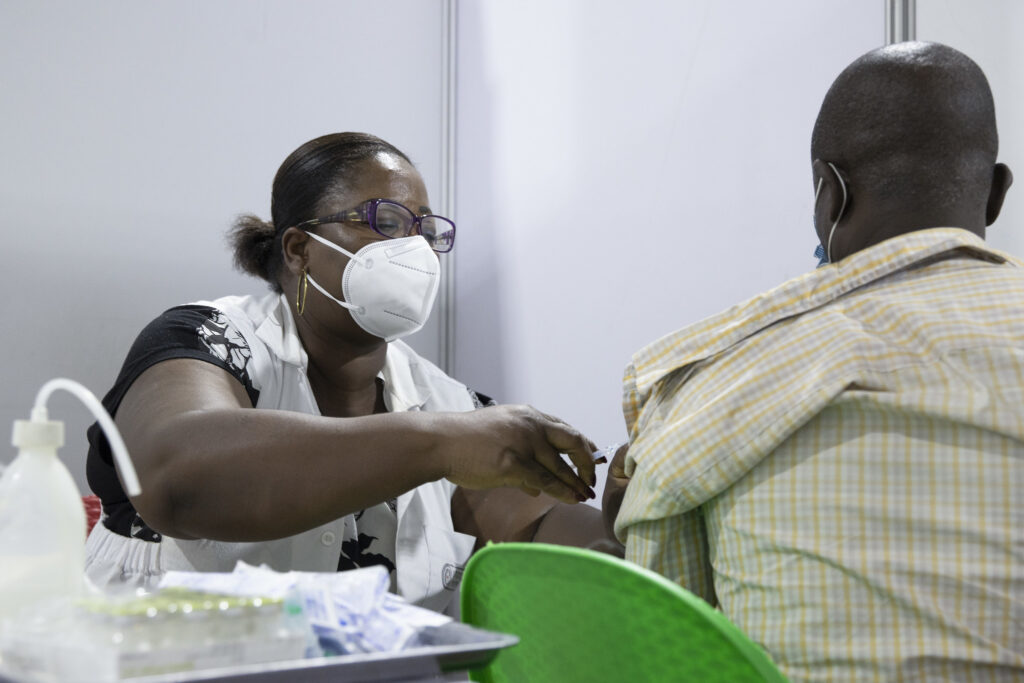
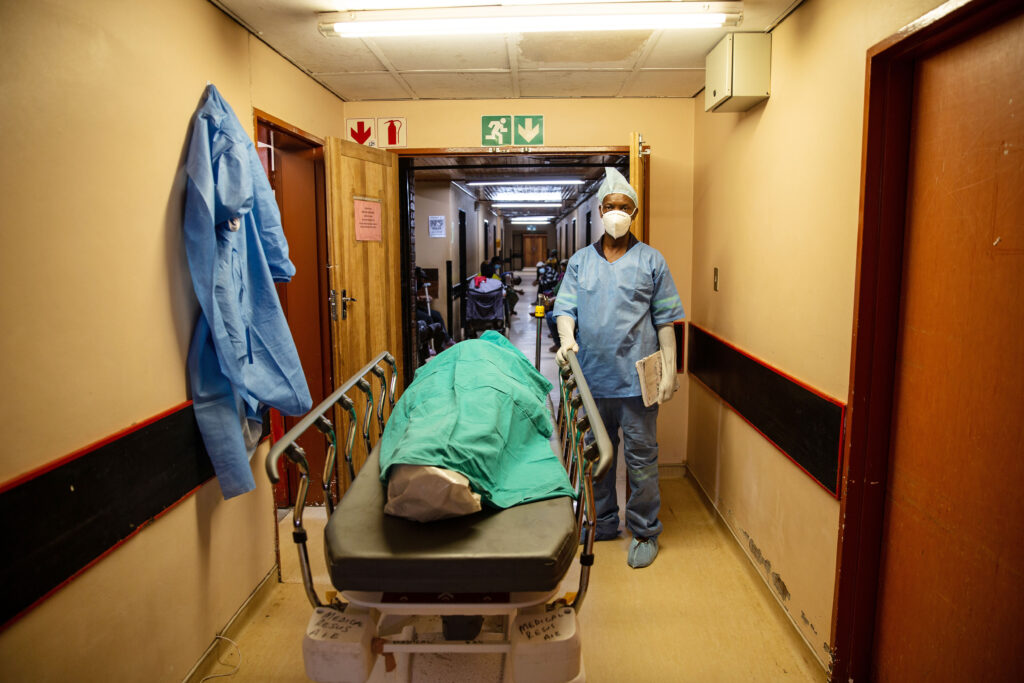
- The list of medicines that South Africa’s professional nurses can prescribe to patients hasn’t changed since 1984, which means their permissions stop at schedule four drugs (which includes antivirals and antibiotics).
- The health department got close to updating these rules in 2011, but didn’t follow through.
- Real change will have to happen soon though since South Africa’s new five-year strategy to curb HIV and tuberculosis includes a plan that would require professional nurses to prescribe medicines to treat anxiety, depression and substance use disorders. The state plans to be able to treat about a quarter of a million people for these conditions by 2028.
Over the past twelve years, three consecutive South African health ministers have failed to update the rules that govern which drugs professional nurses are allowed to prescribe to patients — even though they didn’t have to go through parliament to do it.
Draft regulations that would let trained professional nurses prescribe and dispense schedule 5 and 6 medicines were published back in 2011 to get feedback from the public. All that remains is for the changed rules to be signed off, according to pharmacy and regulatory expert Andy Gray. He was speaking at a Twitter Spaces event hosted by Bhekisisa on 5 April.
Medicines are classified in a schedule (levels 0–8) according to how likely they are to make a person become dependent. The higher the schedule of a medicine, the more careful doctors and pharmacists have to be when giving it to patients, and the stricter the rules are about how much of the medicine someone can get at a time.
Medicines such as antidepressants are grouped under schedule five and the prescription schedule for narcotic painkillers such as morphine is one level higher. Medicines at these levels have a moderate to high risk of dependence and so they can only be prescribed by doctors at the moment.
Because Aaron Motsoaledi, Zweli Mkhize and Joe Phaahla all failed to complete the final steps required for the new regulations to kick in, South African nurses’ prescribing rules are stuck in 1984, when they were first published.
In practice, this means nurses can be trained to prescribe and dispense medicines only up to schedule four (which includes antibiotics and HIV treatment, for instance).
But real change may have to come soon.
South Africa’s new five-year (2023–2028) strategy to fight HIV, tuberculosis (TB) and sexually transmitted infections includes a plan to train professional nurses to prescribe a host of schedule five and six medicines under the supervision of a doctor, such as drugs to treat anxiety, depression and substance use disorders.
The health department aims to have enough antidepressants or drugs for substance use disorder available in the public health sector by 2028 to help over 250 000 people who need these medicines.
It’s part of a bigger plan not only to bring mental health services to primary care facilities so that it’s easier for someone to get support for psychological conditions, but also to curb HIV and TB infections.
Anxious and depressed people are more likely to get infected with HIV and TB since they might engage in risky coping mechanisms such as unprotected sex (which can lead to HIV) or smoking (which can make it easier for a TB infection to get out of hand).
The outdated prescription rules, however, aren’t the only problem that could complicate how nurses can help to improve South Africans’ quality of life.
Nurses move around often. Their prescribing permissions don’t
A project called Nimart, which is short for Nurse Initiated Management of Antiretroviral Treatment, has allowed South Africa’s professional nurses to prescribe antiretroviral medicines (ARVs) to manage HIV treatment, after they’ve completed special training.
Before this project kicked off in October 2010, only doctors were allowed to prescribe ARVs. But from 2010, South Africa’s HIV treatment rules expanded so that more HIV-positive pregnant women, infants and TB patients could get ARVs. That meant that public sector doctors needed extra hands to help with prescriptions.
Nimart-trained nurses helped to relieve the pressure quickly.
A tracking study in Johannesburg to assess the impact of the programme showed that in the year before Nimart started, people who tested HIV positive could get treatment from only one of the 17 clinics studied and all prescriptions were from doctors. Twelve months later, all 17 these facilities were able to give their patients ARVs because nurses were able to help with prescriptions. As a result, an average of 732 patients were started on treatment every month in the year after the new system kicked in, up 26% from the monthly average of 580 people the year before.
By handling many of the more straightforward HIV cases, the Nimart nurses were also taking pressure off referral hospitals, which allowed the doctors there to get to patients with more complicated situations, the researchers explain.
Moreover, a 2014 evidence review found that the quality of care patients can expect when nurses manage their HIV treatment is similar to what a doctor is likely to give.
Despite the positives, Nimart has some hiccups.
Nurses’ permission to prescribe and manage ARVs is linked to the facility where the person works when they apply, so they lose their prescribing rights when they move to another clinic, Juliet Houghton explained to the Twitter Spaces audience. Houghton is the chief executive officer of the Southern African HIV Clinicians Society.
Nurses move around between facilities often, she says, either because they’ve found a better job or because they’ve been promoted to a higher position elsewhere.
Will SA clinics be able to bridge the support gap?
Permission problems aside, lacking mentorship for nurses from clinic managers can hinder how effective Nimart is, researchers write in a 10-year review of the programme in the Southern African Journal of HIV Medicine.
A lack of supervision and support from managers means nurses lose confidence in their ability to turn their training into practice, and so they become less effective at starting and keeping people on ARVs.
A study of 101 primary health facilities in rural North West found that even though three-quarters of professional nurses in nearly all of the clinics (99%) in the study had Nimart training, the number of people who stayed on their medicine and took it correctly (and so managed to get their viral count so low that they could not transmit the virus) remained at about 50% across the five years — well below the 90% target. This suggested that the Nimart training had gaps in helping nurses monitor and follow up on their patients, the researchers write.
Still, the doubts that people had about whether nurses would be able to manage HIV treatment have been shown to be unfounded, Houghton says.
“With the right support and training, nurses can help take health services closer to people’s houses, and help them to stick to lifelong treatment.”
Mental health support is about more than pills
To diagnose if someone has HIV only takes a blood test, but determining whether somebody has depression, anxiety or a substance use disorder is far more complicated, Gray explained during the panel discussion, because people’s experiences of these conditions can vary.
Yogan Pillay, a clinical psychologist who leads the local arm of the Clinton Health Access Initiative, warned that not everyone struggling with a mental health issue will need — or want — to take pills, so other kinds of support must be available as well.
In the long term, the government will have to address the societal problems that people are dealing with, such as unemployment, to improve citizens’ quality of life — and by extension their mental health, he says.
“If someone is depressed because they’re unemployed, giving them antidepressants will make them feel better for a while, but it won’t fix the problem,” Pillay noted.
More pressure on SA’s all-rounder nurses
The health department doesn’t buy antidepressants and medicines to treat substance use disorders for primary health clinics at the moment, because nurses aren’t allowed to prescribe and dispense them, according to Gray. He serves on the committee that decides which medicines the state should buy for the public sector, called the National Essential Medicines List Committee.
If South Africa’s nursing laws change and the health department does start to buy these drugs for clinics, it’s likely that professional nurses will have to play the role of pharmacist as well, Gray argues because there are so few of these health workers in the country’s state sector.
South Africa has one pharmacist for every 3 038 people, the pharmacy council’s 2023 data (though these figures include people who have retired or left the country). Moreover, only about a quarter of them work in the public sector — with the most at facilities in Gauteng, the Western Cape and the Eastern Cape. This number is well below what would be expected in a middle-income country, experts wrote in the Canadian Journal of Hospital Pharmacy in 2016.
Although professional nurses’ permits allow for dispensing only if they’re providing home-based care or if they treat babies (that is, not if they work in a clinic at a pharmacy), the NSP says the government wants these health workers eventually to be able to dispense antidepressants as well.
But to allow nurses to focus on their clinical tasks, Gray says that the state could employ pharmacist assistants to help with prescriptions at clinics and community health centres. This would require further change to the country’s pharmacy regulations since such assistants currently still have to be supervised by a pharmacist.
At the moment nurses working in state facilities have to be jacks of all trades, Gray says, and it’s not sustainable. “Prescribing and dispensing at the same time would put incredible stress onto primary care nurses.”
Joan van Dyk was a health journalist, senior health journalist and news editor at Bhekisisa between 2017 and 2023.