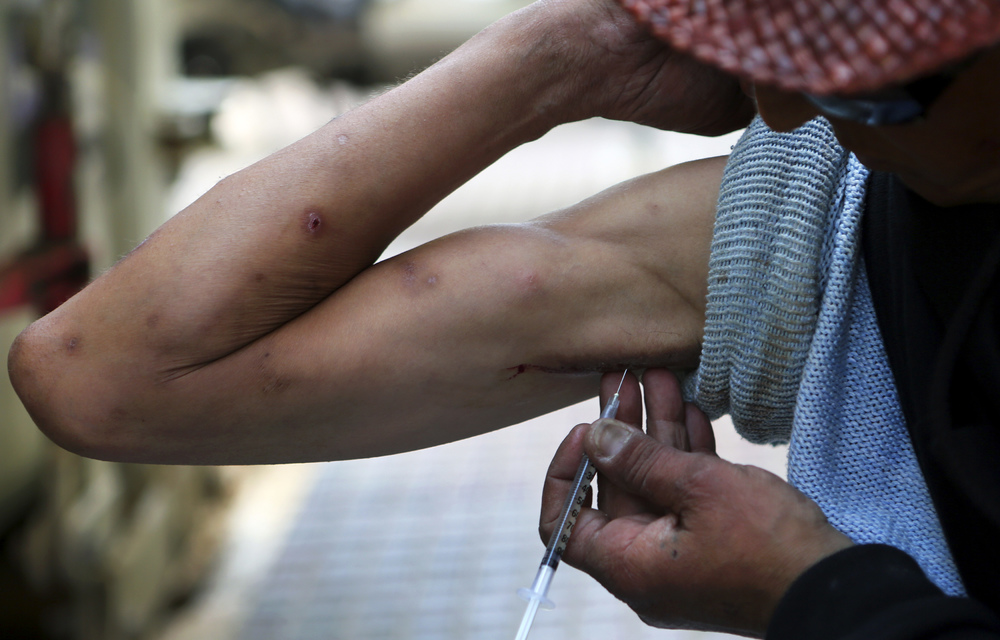
- A study of 31 countries found that South Africa made up a third of all over-the- counter codeine sales between 2013 and 2019. Codeine is found in mild painkillers and cough syrups, and is sometimes mixed with Sprite or alcohol to make a drink called “lean”.
- One in five people in the country experience persistent pain, but experts worry that misuse is driving sales as well, particularly among young people. More and more adolescents are showing up at drug treatment centres to try and kick the habit.
- There are systems in place to monitor codeine abuse at pharmacies, but the loopholes in such safety mechanisms are getting wider, and it’s teenagers that are paying the price.
Kieran Gordon* woke up dazed and freezing. He was lying in his underwear on the floor of the living room at a friend’s house in Johannesburg.
Someone was fumbling with keys by the front door, stirring a few of the other party guests still passed out.
Gordon, then 14, couldn’t remember what had happened the night before, but he recalls he saw chips packets and about 20 empty two-litre bottles of Sprite scattered on the ground.
He patted around him, searching for his clothes. The only thing he found was a half-full styrofoam cup, and there wasn’t time to look any further.
“What’s going on here?” an angry female voice suddenly demanded. Gordon’s friend’s parents were back home.
“What’s this purple stuff?” his friend’s mother wanted to know.

Gordon sat up and scanned the room. His vision was blurry, he recalls, but on the kitchen counter next to some Sprite, he could see what looked like about 10 cough syrup bottles.
They had all been drinking “lean” the night before, a typically purple drink made by mixing alcohol or a soft drink with codeine-containing medicine such as cough syrup. It also commonly goes by the name purple drank or sizzurp.
Codeine is a mild painkiller of the same type as morphine, called opioid drugs. Opioids make your brain release feel-good chemicals and it doesn’t take too much to get to a drowsy, pleasurable high. Which is exactly what mixing 100ml of codeine-containing medicine with two litres of soda does.
No one else responded to his friend’s mom so Gordon fumbled for an excuse and said: “The cool drink must be expired, ma’am.”
“A pharmacy is not a kiosk”
Nine years since Gordon, now 23, had his first cup of lean, he struggles to kick the habit. Sitting in his car in a parking lot at the Rosebank Mall in Johannesburg, he watches shoppers mill in and out of the centre, getting last-minute supplies for the week ahead.
He pours the cough syrup into a cup of Sprite, sits back and takes a sip as the air fills with a potent blackcurrant smell.
It’s a trap that’s difficult to escape, because opioid drugs such as codeine, morphine and heroin are addictive and over time your brain needs more and more of it to get the same high.
“It was unlike anything I’d ever tasted before,” Gordon says of his first lean experience.
The drink had a lingering aftertaste, and a numbing sensation that started on his tongue before spreading to the rest of his body.
And a 2020 study among 144 schoolchildren aged 14 to 17 from two townships in Mpumalanga and the Free State, shows that South African teenagers are similarly enchanted.
[WATCH] Chasing the dragon, stalking a virus: Life, heroin and Tshwane’s needle exchange
Some young people told researchers they first saw people using lean on social media: “Anything that is trending on Instagram is the one that we’d like”.
Adolescents are particularly vulnerable to addiction as the part of the brain that controls rational decision-making is not yet fully developed. Getting hooked on drugs early in life can also lead to long-term dependence and psychiatric disorders such as depression later in life.
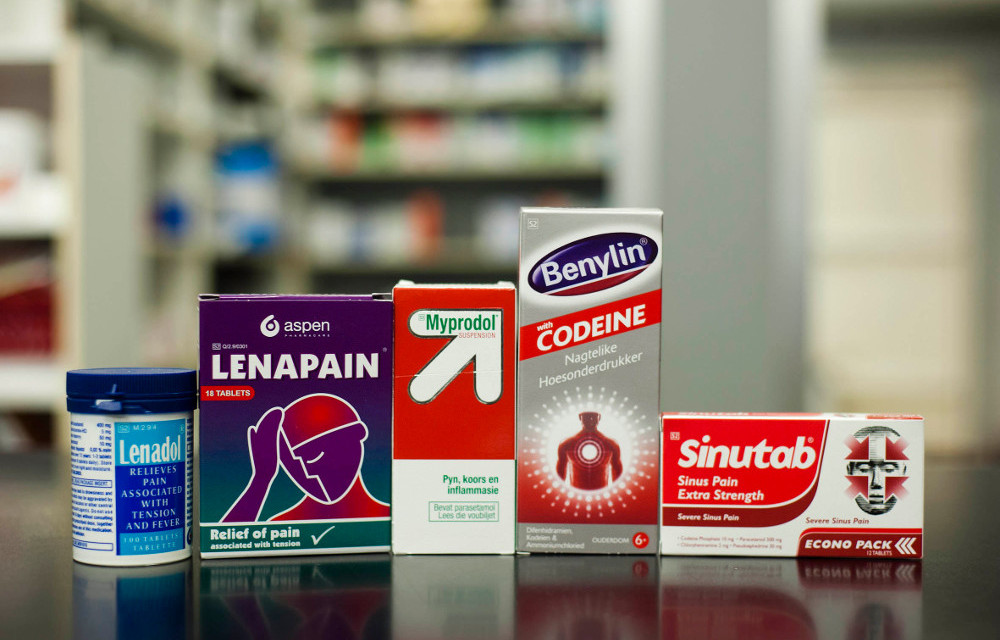
A codeine high comes not only cheap (R20-R30 for a 100ml bottle of the pain medication Stilpane or cough syrup Broncleer plus R20 for a bottle of Sprite), but also easy.
These medicines are available over the counter at pharmacies — with little oversight of who buys them, as Gordon can attest.
The day after his first taste of lean, Gordon walked to a chemist in his school uniform, asked for a 100ml bottle of Broncleer, and got it. Teens who participated in the local study on cough syrup misuse reported that “you just go to the pharmacy and buy”.
While it’s mostly codeine-containing syrups being misused, tablets have as much potential for abuse. In a study on codeine abuse in South Africa, a third of the participants reported abusing codeine tablets such as Stilpane and Adcodol.
But it shouldn’t be that simple, says Mariet Eksteen, professional development officer at the Pharmaceutical Society of South Africa.
Broncleer and Stilpane syrups are Schedule 2 medicines in South Africa because they contain little enough codeine to be safe if used as intended. The higher the schedule of a drug is, the more restrictions there are on how and when it can be dispensed.
But even though Schedule 2 medication can be bought over the counter without a doctor’s prescription, the dispenser must record the name, ID number and address of the person it was sold to.
(Codeine on its own is a Schedule 6 drug, because of its potential for addiction if used at more than 20mg per dose).
Still, a pharmacy is not a kiosk, Eksteen says.
Pharmacists are supposed to make sure patients know how to use self-administered medicines safely. “You don’t just hand it over.”
In the parking lot at Rosebank Mall, Gordon puts down the bottle of Stilpane he’d been holding. There’s another in the cupholder between the seats and two more in the passenger door pocket.
He stares out the window and says: “I’ve never signed any [log] books.”
Listen to Zano, on the Afternoon Drive with John Maytham, as he discusses the misuse of codeine amongst our youth.
For the (lack of) record
Research across 31 countries found that South Africa (the only African nation in the study) accounted for almost a third of all over-the-counter sales of codeine, almost one and a half times as much as the second highest consumer, France, between 2013 and 2019.
So where is it all going?
Many people are, of course, buying these medicines because they’re in pain — nearly one in five people in South Africa experience constant discomfort, mostly in their backs and limbs, reports a 2020 study of more than 10 000 people.
But, health professionals and regulators worry that the amount of codeine consumed in South Africa isn’t all for legit uses. And, says Daphney Fafudi, manager of regulatory compliance at the South African Health Products Regulatory Authority (Sahpra), their data shows that most of the misused codeine products come from pharmacies.
Sahpra is the country’s medicines regulator and it tracks every batch of codeine-containing painkillers from when it’s made to when it’s sold.
The body does this by, for example, taking stock at the manufacturers and wholesalers to ensure what comes in tallies with what goes out and dropping in on randomly selected pharmacies to check their orders for codeine-containing products against stock in store and sale records.
That’s how they noticed something dodgy happening at some dispensaries in 2019. “You wonder [why] when a person should be getting one bottle, the establishment is giving a box or more than one box,” says Fafudi.
Not only was codeine being sold in bulk, some pharmacies were not recording the details of the people they sold the products to, she adds.
But it doesn’t seem to be pharmacists as such who are dishing out codeine indiscriminately; instead the issue seems to be at outlets where there’s no pharmacist on duty.
In 2019, the South African Pharmacy Council investigated 14 chemists nationwide for allowing unauthorised personnel to do things only a pharmacist should, such as dispensing over-the-counter medication and offering health advice to patients. This was the highest number of this sort of contravention in five years.
More and more codeine-dependent teenagers are also beginning to show up at South Africa’s drug treatment centres, says Siphokazi Dada, a researcher formerly at the South African Community Epidemiology Network on Drug Use. In 2016, about one in five people admitted for codeine dependency was between 10 and 19 years old; by 2019, this number had jumped to about one in three.
When a fix can break you
One day, when Gordon was about 16 years old, he was at home trying to make a stronger drink of lean. Instead of adding just one bottle of the syrup, he poured two into two litres of Sprite — essentially double strength.
After a few moments, he realised he would have to lie down.
He realised he had accidentally overdosed: “I couldn’t talk. I felt paralysed. I couldn’t even feel my heartbeat,” he remembers.
Overdosing on codeine can cause damage to the respiratory system and kidneys, as well as unconsciousness, a weak pulse and slow heartbeat.
The incident, however, didn’t slow Gordon down. He kept drinking about four litres of lean every day, which amounts to swallowing about 14 bottles — close to one and a half litres — of cough syrup a week. The safe maximum adult daily dose for over-the-counter codeine is 80mg. A full bottle of cough syrup can contain up to 200mg of codeine, so Gordon, as a teenager, could consume as much as 400mg of the drug a day, five times the recommended safe dose in this form.
Gordon’s codeine habit messed up a lot of things in his life.
“I almost failed grade 11. I couldn’t study while I was on lean; my mind wasn’t right. I couldn’t fall asleep without it,” he says.
His relationship with his parents also took strain. His mother once found about 30 empty bottles of Stilpane in a bag in his cupboard and threatened him with rehab.
So he decided to “put his head down and stop for a while”. But it was difficult to regain his parents’ trust.
He smirks for a second and says: “If I poured myself a glass of cold drink my mother would throw snide remarks like, ‘What’s in that cup?’”
A possible solution — with some loopholes
To try and curb the abuse of codeine and so help prevent opioid misuse from becoming an epidemic as in the United States (US), the Pharmaceutical Society of South Africa and other partners launched the Codeine Care Initiative in 2013.
In the US, opioid abuse is so common that it’s contributed to a small drop in how long people in that country are expected to live. In 2018, about three in 100 adolescents and 5% of people between 18 and 25 in that country reported misusing opioid pain relievers.
When it was first launched nine years ago, the Codeine Care Initiative was supposed to be a national database where pharmacists would be able to see every codeine purchase someone has made in the last six months, regardless of which pharmacy chain they visited.
But because the project wasn’t mandatory, only about 10% of drug stores in the country opted in, according to Eksteen.
As the medicines regulator, Sahpra has the power to make sure a system like this is uniformly implemented in pharmacies nationwide, she says, which could help to put an end to “pharmacy hopping” (when someone skirts suspicion by going to lots of different outlets to get their fix).
[WATCH] Magic methadone: ‘Getting clean is the easy part, staying clean is the hard part
If the system alerts a pharmacist to a customer who’s been using codeine products regularly, they’ll be able to talk to them about the risks or suggest a medicine that doesn’t contain the drug. Dispensers can also refuse to hand over a medicine if they think it’s in the patient’s interest to do so.
Most states in America have similar databases, called prescription drug monitoring programmes, for medicines that carry a high risk of dependence, such as the pain medication oxycodone.
Says Eksteen: “Having a system like this is an opportunity to say: ‘Do you need help? Can I advise you on a different product?’”
Upscheduling vs. monitoring
Making codeine-containing medicines available only on prescription is another option, which countries such as France and Australia have gone for. In Australia, upscheduling the products led to almost 90% fewer sales of low-dose codeine medicines in the next year and cut the monthly number of overdoses by half.
Sahpra has considered changing the schedule of the products here too, but local experts advised that monitoring the sale of codeine-products would be a better route for South Africa because a change in scheduling would put the painkiller out of reach for people who can’t get to a doctor easily.
Eksteen says the pharmaceutical industry, healthcare professionals and regulatory bodies will, however, have to pull together to make this work.
Why?
For one, because there’s no guarantee that the outlets will use the system. Participation is voluntary and the products tend to be channelled to misusers from community pharmacies with unauthorised personnel. Evidence from the US shows that even prescribers who are authorised to give out these medicines don’t use monitoring systems often.
The Protection of Personal Information Act could also complicate getting South Africa’s database running. Because the act requires organisations to get people’s consent for storing their personal information, the Codeine Care Initiative will require permission from the customer to take part, explains Eksteen.
So if someone’s planning to misuse the medicine, they’re unlikely to allow their purchasing record to be saved. In this case, the pharmacist may still note on the registry that the patient declined to participate, but without any details as to who the customer was.
Research from the US also shows that pharmacies in rural areas were less likely to participate in an online prescription drug monitoring programme than those in cities or large towns. But an even bigger factor for not using the system was not having internet access.
Only one in five workplaces in rural areas has internet access in South Africa.
Many users have already noticed loopholes like these, including Gordon.
He explains: “I just go down to the [smaller] pharmacies. If I go to [the ones in malls], I’d get denied. Those ones are a last resort.”
These days, Gordon allows himself a cup of lean only when he’s got something to celebrate.
“I know that I can’t do this forever. I want things to happen for me in this life. I can’t let lean distract me like it did in high school.”
*Kieran Gordon is a pseudonym