This silent killer stalks expecting mothers around the world and is one of the leading causes of maternal mortality in South Africa. But still, many women can’t name it — or identify its symptoms. But if knowledge is power, is it enough to stem this deadly tide? Ghana is hoping to find out.
The sun was beginning to set but still, the painkillers had done little to soothe the throbbing pain in Koiwah Koi-Larbi Ofosuapea’s head.
At their home in Accra, Koiwah’s husband, Dennis, tried to comfort her.
He was worried, but careful not to show it.
“Don’t you think the headaches, the tiredness, the fatigue is just part of the pregnancy?” he tried to comfort her.
“Maybe,” Koiwah nodded.
But she didn’t really know.
Her first pregnancy had been anything but easy.
But she’d been for all her antenatal check-ups at a private clinic. At six months’ along, not one nurse or doctor said she had anything to worry about — not even when she mentioned the pounding headaches.
The pain in her head bothered her. But what was she supposed to do about it?
About an hour after the sun had gone down, when dusk was slowly falling over the jostling city, Koiwah and Dennis turned in for the night.
Nearby, stacks of baby clothes lay ready to welcome what scans suggested would be the couple’s new daughter.
But at 2am, Koiwah’s body began to shake viciously jarring Dennis awake.
“Koiwah! Koiwah!” he screamed, grabbing her.
It was the last thing she heard before she lost consciousness.
‘For three days, I bathed and cleaned him. We had this bond’
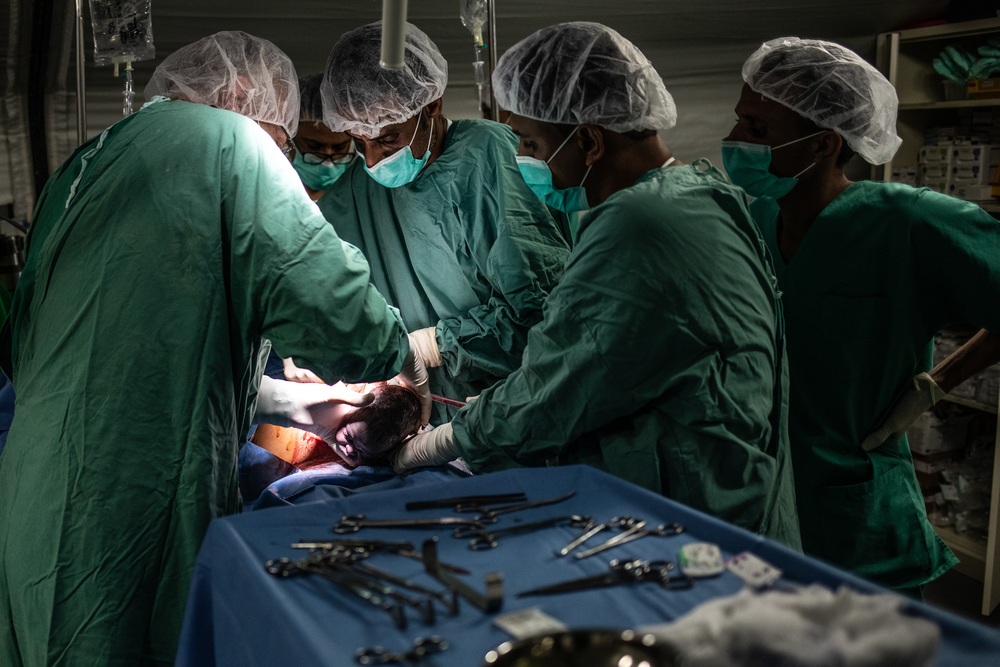
A day later, Koiwah awoke in a hospital bed.
Her baby was gone.
“I was in so much pain — I’d had an emergency cesarean section,” she remembers.
In a YouTube video she made about the incident, she explains the doctors had diagnosed her with something she had never heard of: eclampsia.
Preeclampsia is a condition that happens during pregnancy that causes women’s blood pressure to soar. It can damage organs, most often the kidneys or the liver, explains the US health research organisation Mayo Clinic. Although the illness can develop without warning signs, women often experience symptoms such as shortness of breath, blurry vision and headaches just like Koiwah.
“When preeclampsia isn’t controlled, eclampsia — which is essentially preeclampsia plus seizures — can develop,” the nonprofit cautions on its website. “Because eclampsia can have serious consequences for both mom and baby, delivery becomes necessary, regardless of how far along the pregnancy is.”
Scientists aren’t sure what causes preeclampsia, but it may have something to do with the placenta, Mayo Clinic says. Early in pregnancy, new blood vessels develop to make sure the placenta, which nourishes the fetus, has an adequate supply of blood. But in women with Koiwah’s condition, these blood vessels don’t seem to develop properly. This could be due to a family history of the condition or problems with the immune system. Koiwah’s mother had preeclampsia with five of her pregnancies.
Koiwah spent days in hospital waiting for her blood pressure to drop.
To her surprise, the baby scans had been wrong.
She’d had a boy. Because he had been born prematurely — in the sixth month of her pregnancy, he was struggling to breathe and had been admitted into the hospital’s neonatal intensive care unit (ICU).
When Koiwah became strong enough, she would go to the ward to wash her son.
She remembers: “He was so little, less than one kilogram.
For three days, I bathed and cleaned him. We had this bond.”
On the sixth day Koiwah was well enough to go home. Her son, however, wasn’t. But, hospital staff assured her, she could come to feed and wash him every day.
But when Koiwah and Dennis arrived at their son’s ICU bed the next day, he was gone. A nurse told them he had been transferred.
“I knew something was wrong,” she Koiwah recalls. “We were asked to leave and come back the following day.”
On the way home, Dennis’ cell phone rang. He took the call and then hung up.
Dennis took a deep breath. Then he turned to Koiwah and softly said: “We’ve lost the baby.”
‘I’m only a little bit above 30 and already I have lost two children’
Her son’s tiny body and face on the last day that she had seen him is etched in Koiwah’s memory.
But it wasn’t the end of her trauma.
Preeclampsia is just one of several complications related to high blood pressure — collectively called hypertension disorders — that can happen during pregnancy. Disorders like these accounted for 14% of deaths among women during pregnancy, birth or shortly after in roughly the last decade, a 2014 review published in The Lancet shows. In Africa, this percentage was slightly more: high blood pressure contributed to almost two out of every 10 maternal deaths.
Back in Ghana, just as the rainy season was about to set in, Koiwah was pregnant with her third child — a boy.
It was 2017, five years after her first pregnancy and in the meantime, she and Dennis had already welcomed a daughter.
But now, in the sixth month of pregnancy, she started to feel something was off.
At the hospital, doctors couldn’t find the fetus’ heartbeat. And — again — Koiwah’s blood pressure was dangerously high.
“I had to wait two days more to get the dead fetus out,” Koiwah she writes in a blog. “Such pain I had to go through with no compensation of a baby to heal my wounds.”
She adds: “I’m only a little bit above 30 [years old] and already I have lost two children.”
Ghana, like South Africa, has struggled to bring down high rates of maternal mortality. In fact, in 2017, the number of women who died per every 100 000 live births in the West African country was almost double that of South Africa, data from the United Nations Children’s Fund shows.
There are no national statistics for how many women develop preeclampsia each year, but studies using data from some of Ghana’s biggest hospitals have shown that the condition may account for between 30 to nearly 50% of admissions for hypertensive disorders. Meanwhile, the number of maternal deaths from these conditions doubled between 2007 and 2017, shows the latest maternal health survey.
In South Africa, these kinds of illnesses were the second leading cause of maternal deaths in 2016 — behind non-pregnancy related infections such as HIV and TB, the country’s audit of maternal deaths shows.
And the problem is growing. Deaths attributable to hypertensive disorders increased by 14% between 2011 and 2016.
From clinic to hospital: It’s a rocky road of referrals for women on death’s door
In Ghana, the Komfo Anokye Teaching Hospital is the country’s second-biggest hospital and serves half of the country’s 10 northern regions. Here, preeclampsia accounted for one in two admissions for hypertensive disorders in the second half of 2014.
More than 80% of the hospital’s cases of hypertension disorders among pregnant women were referred from other smaller facilities that lacked the equipment or know-how to save mothers and their babies. In some cases, women had to self-refer themselves, researchers in a study published in the journal PLoS One wrote earlier this year.
A lack of transport between clinics and hospitals was thought to be a factor in almost two out of every 10 deaths in South Africa from conditions like preeclampsia. In almost a third of such cases, it’s thought that a lack of skilled doctors proved deadly.
In Ghana, even large hospitals may be struggling to provide quality care for women like Koiwah. For instance, when scientists evaluated how well doctors and nurses stuck to treatment guidelines in a large regional hospital in Accra, they found mixed results. Only half of women with preeclampsia who needed it received the mineral magnesium sulphate as per protocols to reduce the risk of seizures. A 2014 PLoS One study shows this percentage fell even further when it came to administering the drug hydralazine to control blood pressure.
Researchers found that staff were better able to stick to the rules if they’d received recent training or if there were signs around the hospital to serve as a reminder. Assigning people tasks upfront — such as dispensing a certain type of medication — also meant it was more likely to get done. But neither of these was enough to protect women from what scientists pointed out were occasional medication stockouts, staff shortages or breakdowns in equipment.
Even at the massive Komfo Anokye Teaching Hospital in northern Ghana, a lack of equipment could explain why the facility has a higher death rate among newborns born to women with eclampsia than similarly large hospitals with higher premature delivery rates in countries like Canada.
Koiwah, who delivered a daughter she named Deoli abroad, saw the difference first-hand.
“In the United States, where my daughter was delivered, there were lots of machines that did 24-hour monitoring,” she says. “Where you live could determine whether you’ll be alive or not.”

It’s lunchtime in bustling Accra.
On the city’s busy Legon E Road, white minibus taxis stop and go, collecting and dropping passengers as workers in search of a meal cross the wide avenue via an overhead bridge.
Not far from the main road, Koiwah is at her office where she settles into a chair and sets up her mobile phone. Then she switches it to camera mode, takes a breath and hits record.
“Hello everybody,” she says.
From below the camera’s frame, she produces a grey book. On its cover, stands a heavily pregnant woman next to the words, “Understanding preeclampsia”.
She continued: “Many of you know me, some don’t but that doesn’t matter. We are here with an agenda to educate and save lives.”
In the video, she tells her audience that this is the first in a six-week Facebook seminar based on the book where, together, they’ll try to understand the questions women have about the condition.
The series is sponsored by Action on Preeclampsia Ghana — an organisation Koiwah started initially as a campaign in 2017 to raise awareness about the condition. But two years later, it’s taken on a life of its own, becoming a non-profit organisation and partnering with similar international initiatives.
She may not be able to keep medicines in stocks or fix staff shortages, but Koiwah does think she can help empower women to know the signs of preeclampsia in hopes they can get better treatment earlier. Raising awareness like this — in tandem with better access to safe c-sections — is just one of the ways South Africa is also hoping to curb deaths among pregnant women here at home.
Traditionally, doctors and nurses globally have used high levels of blood pressure and protein in the urine to diagnose women with preeclampsia in their second or third trimesters.
But 2016 research published in the American Journal of Obstetrics & Gynecology suggests the condition could be picked up much sooner. As part of the study, scientists looked at the medical records of more than 35 000 pregnant women in the United Kingdom. They found that if doctors looked at women’s medical history of risk factors — such as diabetes or obesity — and also ran a selection of tests to detect more detailed blood pressure rates within, for instance, the uterus, and protein levels linked with the development of the placenta, they were able to accurately predict 75% of early and more complicated preeclampsia cases.
But not all the tests used in this kind of screening are widely available, the researchers note, especially in resource-poor countries.
What could save mothers in countries such as Ghana and South Africa in sub-Saharan Africa?
A 2015 study plugged existing research about a range of possible solutions from increasing diagnoses to c-section to providing women with magnesium sulfate. Magnesium sulfate is used to prevent seizures in women with preeclampsia or eclampsia as well as to stall premature delivery for up to two days to allow doctors to treat women with these conditions.
The research found that diagnosing more women with the condition and getting them to hospitals where doctors can perform c-sections or induce labour would save the largest number of lives. Whether or not women got magnesium sulfate only showed a very small benefit when it came to reducing overall deaths, the research, published in the journal Obstetrícia et Gynecologica Scandinavia, found.
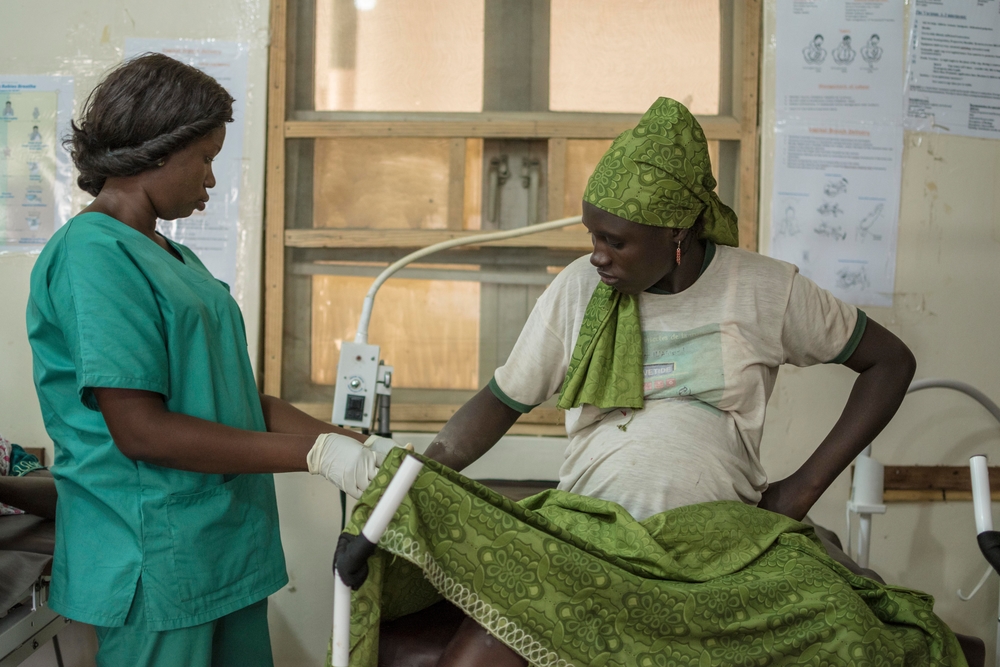
Koiwah’s organisation has regional coordinators — the majority of whom are nurses or midwives — who identify high-risk pregnant women to help increase the number of women who are diagnosed with preeclampsia. So far, they’ve found more than 250 women at high risk of the condition and referred them to obstetrics and gyneacology specialists who are within the organisation’s network for care.
In the future, Koiwah says she wants to provide women with home blood pressure monitors. Although a handful of studies suggest that this could help women monitor their blood pressure and reduce burdensome clinic visits for the routine test, scientists suggest that larger, stronger studies are needed to understand how well this really works.
And when researchers compared how many at-home machines had been tested for accuracy among pregnant women, almost a third lacked a thorough review, according to a 2018 study in the journal, Hypertension. Take home pee tests for preeclampsia, meanwhile, are still in early phases of development, caution researchers in a study published earlier this year in The Lancet’s EClinicalMedicine journal.
Back in Accra, Kowiah is finishing off her weekly Facebook live discussion.
“Now it says that diseases in pregnancy attract less funding than big diseases such as cancer or heart disease or diabetes,” she says, still quoting from the big grey book.
A comment pops up below the feed:
“My experience was terrifying,” writes Juliet Naa Ad Ankamah. “A lot of women do not know about it — spread the word! God bless you, dear.”
As the feed concludes, Kowiah looks up to the camera: “Now, this is very interesting. In other words, funding for pregnancy complications including preeclampsia is less accessible.”
She concludes: “It’s not to say that one is better or worse than another, it’s just to say that everyone should be given attention.”
Gideon Yeboah is a freelance journalist based in Accra. Yeboah writes on a wide range of topics including science as well as arts and culture. Follow him on Twitter @AfroKwabena.
