The World Health Organisation prequalified Merck’s vaccine for widespread use in November but regulatory hoops are just a small part of the fight to get the jab to the places that need it most.
COMMENT
When the US Food and Drug Administration approved the new Ebola vaccine Ervebo last month, I was elated. Ervebo can generate a quick immune response after a single dose, with protection occurring within 10 days.
If only such a vaccine had existed a few years ago, I thought.
In 2015, I co-led an African Union-commissioned evaluation by EpiAFRIC of the AU’s efforts to address the Ebola outbreak in Guinea, Liberia, and Sierra Leone. For two weeks, my team and I travelled throughout the three countries, interviewing AU volunteers, community members, international partners, senior managers at health ministries, and other stakeholders who worked to stem that outbreak. We also visited a Coyah Ebola treatment centre in Guinea.
[WATCH] How an experimental vaccine went from possibility to reality in a time of crisis
During our evaluation, we saw the devastation caused by Ebola, and how weak health systems in the three worst-affected countries had enabled the infection to spread like wildfire. By the time we had finished our interviews, it was clear to us that a stronger health system could have prevented the outbreak, and could even have helped to stop it once it had begun. We wished there was an Ebola vaccine.
Now, there is one.
Without doubt, Ervebo could be a game-changer in tackling future Ebola outbreaks. But, in order to help protect health workers and communities, the vaccine must be delivered safely, sustainably and equitably. That seems unlikely in many countries where Ebola is endemic, owing to security, systemic and social challenges. Unless these challenges are addressed, Ervebo won’t be effective.
When health and insecurity collide
First, without security, Ervebo will effectively be unavailable.
The recent deaths of health workers in Africa, and the derailment and episodic suspension of the Ebola response in the Democratic Republic of the Congo, underline why security is imperative in health-care delivery.
In April 2019, for example, Richard Mouzoko, a World Health Organisation epidemiologist, was killed in an attack on the Butembo University Hospital in the DRC. In 2013, nine female vaccinators engaged in the global polio eradication initiative were killed in two separate shootings at health centres in Kano, northwest Nigeria. The Boko Haram insurgency in Nigeria’s northeast has derailed polio eradication efforts and set back the country’s prospects of being declared free of the disease.
Governments must, therefore, strengthen national security and work closely with health professionals and security agencies to ensure that health workers and community members are not put in harm’s way.
There’s no vaccine for weak health systems
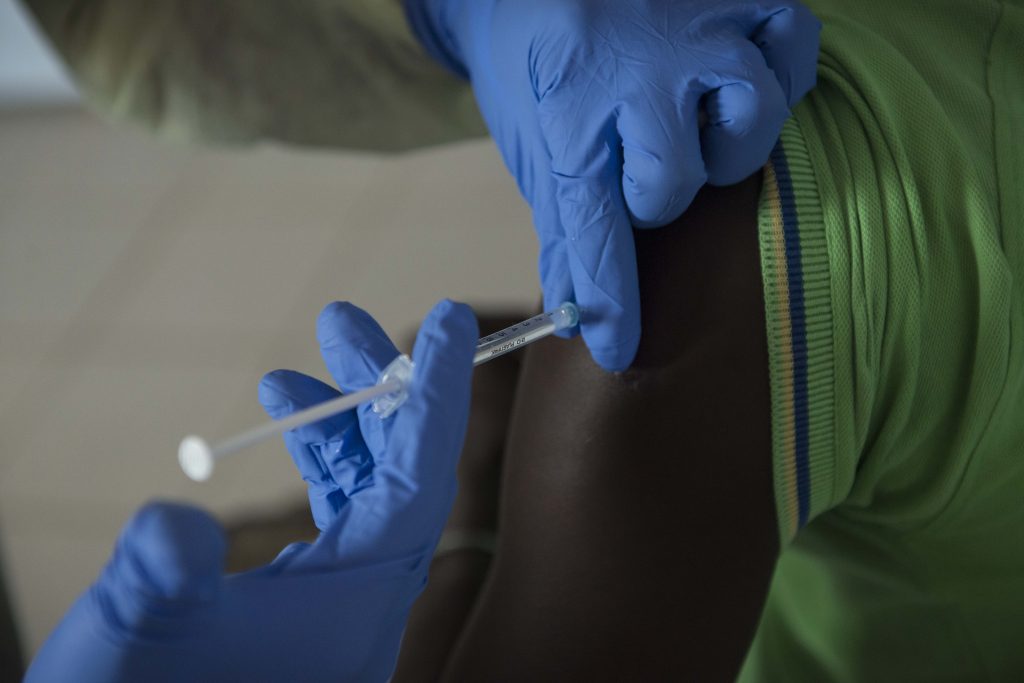
Second, governments must invest in detecting, preventing, and responding to infectious disease outbreaks. According to preventepidemics.org, a website that ranks countries’ epidemic preparedness, no African country currently has the optimal “ready score” of at least 80% on a WHO-supported Joint External Evaluation to perform these tasks.
The five countries that have experienced Ebola outbreaks in the last six years are the DRC (with a ready score of 35%), Guinea (35%), Sierra Leone (43%), Liberia (46%), and Nigeria (46%).
This illustrates the huge challenges that lie ahead: If a country cannot efficiently detect, prevent, and respond to infectious disease outbreaks, how can it know when and where to deploy Ervebo or other vaccines?
Third, it is never too early to explain Ervebo’s benefits to communities before the vaccine is needed. Such efforts should be led by national public health institutes, working with subnational ministries of health and local-government health departments. This is an area in which donors can invest because it amounts to money well spent. Waiting until another Ebola outbreak occurs may delay delivery of the vaccines. Furthermore, past experience has shown that communities have little trust in Ebola interventions in the midst of an outbreak.
Community engagement should also include risk communication, which involves explaining to communities how Ebola is transmitted and what they can do to help prevent outbreaks. The University of Global Health Equity in Rwanda says that “achieving equity in health care depends on equity in health education.” This should be the global health community’s mantra. We should never assume that people know enough about Ebola and other deadly diseases.
Contagion: The ability to contain outbreaks may be determined long before the first case strikes
Finally, we must focus more on the social determinants of health. These factors are usually not considered to be part of the health sector, but they have serious implications for health and health-seeking behaviours. For example, access to clean water and the availability of good sanitation in Ebola-prone communities are vital to preventing and responding to outbreaks and stopping the spread of infection.
Yet, according to the WHO, compared to developed countries, 38% of health-care facilities in low- and middle-income countries lack access to an improved drinking-water source, 19% do not have adequate sanitation, and 35% lack water and soap for handwashing. When health workers cannot wash their hands in clean running water after seeing a patient, they are at greater risk of being infected and of transmitting infections to other patients.
The Ervebo vaccine is a great stride forward in global health.
But while it will save lives, it should not be viewed as a magic bullet for preventing and addressing future Ebola outbreaks.
Above all, international donors must work closely with African governments and national public health institutes to ensure that the vaccine can be delivered to everyone who needs it.
Ifeanyi M. Nsofor, a medical doctor, is CEO of EpiAFRIC, Director of Policy and Advocacy for Nigeria Health Watch, a Senior Atlantic Fellow for Health Equity at George Washington University, a Senior New Voices Fellow at the Aspen Institute, and a 2006 International Ford Fellow. Follow him on Twitter @ekemma.
Copyright: Project Syndicate, 2020.
www.project-syndicate.org
Ifeanyi M. Nsofor, a medical doctor, is CEO of EpiAFRIC, Director of Policy and Advocacy for Nigeria Health Watch, a Senior Atlantic Fellow for Health Equity at George Washington University, a Senior New Voices Fellow at the Aspen Institute, and a 2006 International Ford Fellow. Follow him on Twitter @ekemma.

