- By taking the HIV prevention pill, Tenemine, people can reduce their chance of contracting HIV through sex by 93%. Tenemine is an oral form of pre-exposure prophylaxis, or PrEP.
- The Aurum Institute has been running a PrEP programme in three provinces through their Pop Inn wellness centres, which are aimed at men who have sex with men and transgender women.
- They’ve reached over 100 000 people, some of whom live in some of the country’s most hard-to-reach rural areas.
COMMENT
How would you feel if a nurse held out an enormous blue tablet and said you have to swallow it with water every single day?
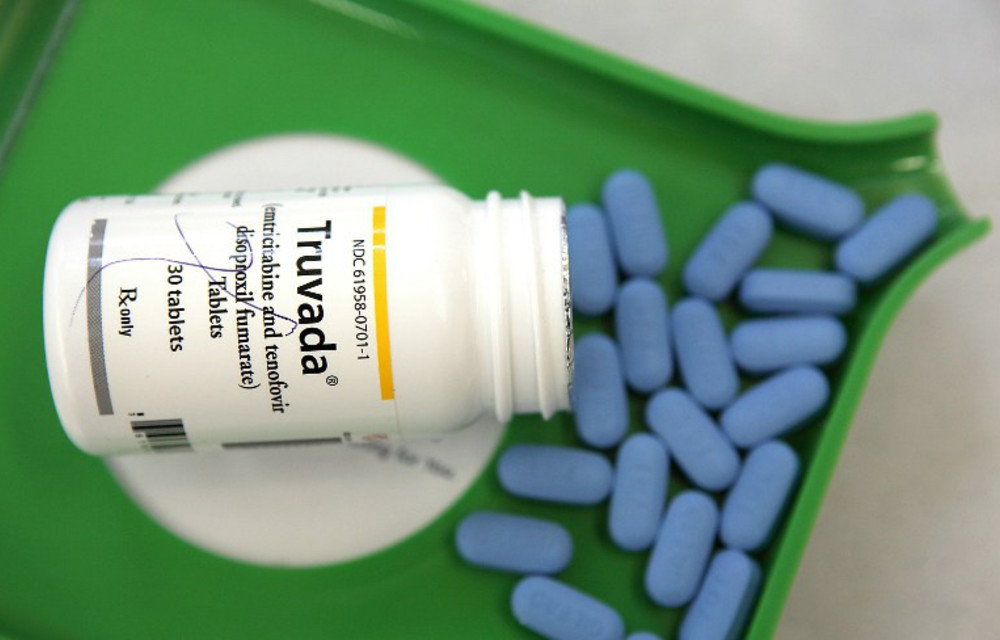
The HIV prevention pill Tenemine (a generic form of the branded drug Truvada) is big and bulky. At nearly 2cm long and almost 1cm wide, it’s about the size of a large jellybean sweet.
The tablet is made up of two antiretroviral drugs (the medicine used to treat HIV) called tenofovir and emtricitabine. If taken daily, the medicine can reduce someone’s chance of contracting HIV through sex by up to 93% studies have shown. Researchers have also found that taking the medication a day before and for two days after sex worked just as well to prevent infection in men who have sex with men and transgender women.
This type of protection is called oral pre-exposure prophylaxis, or PrEP. (So, it’s a medicine you take before you’re exposed to a potentially harmful germ.)
But the high level of protection kicks in only if people actually take the tablets — and stick to it. The less often someone uses the medication, the lower the level of protection becomes.
At the Aurum Institute, an HIV and tuberculosis nonprofit, we’ve been running a PrEP programme at five of our Pop Inn wellness centres in KwaZulu-Natal, Gauteng and Mpumalanga. These facilities are set up specifically for men who have sex with men and transgender women, two groups who are more likely to be become infected with HIV than the general population, partly because the chance of getting HIV from anal sex can be up to 18 times higher than from vaginal sex.
The size of the tablet was one of the reasons people were put off from taking the medicine. By September 2019 only about 8% of people visiting Pop Inn clinics in Ehlanzeni, eThekwini, uMgungundlovu, Tshwane and Ekurhuleni were on PrEP.
But our researchers have figured out how to help people understand that when it comes to protecting yourself against HIV, size doesn’t matter.
Here’s what we’ve learnt.
1. When people are on the move, move with them
Many of the people we help at Pop Inn clinics are migrants. They move around the country or to other parts of Africa for work or to find better jobs.
Migrant workers who have moved between 40km and 110km from their hometowns are 1.5 times more likely to contract HIV than those who don’t move around, a 2017 study in the journal Aids found.
But as people move around more, it also becomes more difficult for them to get PrEP in a convenient way.
For that reason, we’ve set up a partnership to take the service to people when they can’t come to us.
CareWorks is a private courier service that helps people to manage their chronic illnesses by taking HIV prevention medicine, antiretrovirals and self-testing kits to people in hard-to-reach areas.
This partnership has paid off: Since we joined forces with CareWorks in June, 202 of our Pop Inn clients are already getting their PrEP this way.
The service reaches people all across the country, even in places that are way off the beaten track or if someone doesn’t have an official address. In those cases, a person can give the courier a reference point for where they live, such as opposite a specific spaza shop for example.
2. Don’t give a man a fish; teach him how to fish
People often don’t think they’re at risk of being infected with HIV, which means they might not take the right steps to protect themselves. At Aurum, we’ve designed a screening tool to help people figure out how likely they are to get infected with HIV.
PrEP is only useful for people who are HIV negative, so the first thing a client is asked to fill in on the form is what their HIV status is. (They also go for a test later.)
The rest of the questions in the checklist ask how often someone is having sex, whether they use protection such as condoms at all and whether they know their partner’s HIV status.
Once people have filled in all these details, a nurse will sit down with them and explain how HIV infection spreads and what kind of behaviour could lead to a higher chance of getting the virus. The health worker will also give the person an information pamphlet about how PrEP works.
We’ve learnt that giving people the explanations they need to make their own decisions in their own time, rather than just telling them what to do, goes a long way to help them take the medicine. For example, our nurses don’t only talk about the benefits of taking the pills, but also discuss the side effects people may experience when they take PrEP, which can include headaches, tiredness, nausea or bone pain.
The healthcare workers explain what people can do to ease these side effects, such as taking painkillers or getting a check-up at the clinic.
We found that the more knowledgeable people became, the less worried they were about the size of the pill, for instance. We also give them tips on how to swallow it so that it doesn’t get stuck in their throat.
3. Help people to help each other
Our Pop Inn clinics run support groups called adherence clubs. They meet once a month and are led by people who have been on PrEP for a while already. Joining a group like this helps new starters stay on their medicine and encourages them to come back to the clinic regularly to get their pills so that they won’t run out. (It also helps that Aurum covers their transport costs.)
[WATCH] PrEParing to protect yourself: What young people need to know about this free HIV prevention pill
We’ve found that a buddy system works well too. People who belong to the adherence clubs pair up with someone else in the group so that they can remind each other to take their pills or to fetch their medicine from the clinic.
They can also ask our teams questions on WhatsApp or Facebook and make clinic appointments on these platforms.
PrEP to suit people’s sex lives
Since we’ve started explaining to people how they can lower their risk of HIV infection, almost four times more of our clinic users are asking for PrEP. By September 2019, 2 596 people were getting HIV prevention pills from us; today we have 10 305 PrEP clients.
Plus, fewer people are asking for HIV prevention pills you take after possibly having been exposed to HIV, say, during unprotected sex. (This is called post-exposure prophylaxis, or PEP and for the medication to work it needs to be taken within 72 hours of possibly being exposed to HIV — the sooner it’s taken after possible exposure, the better it works.) At our eThekwini clinic, for example, the number of requests for PEP almost halved this year — from more than 50 in 2021 to only 27 in 2022.
[WATCH] Tap, fire, PrEP: Check out the little blue pill that’s been missing from your Grindr game
We’ve also found that many people, especially those who aren’t in stable or long-term relationships, prefer to use “on-demand” PrEP, meaning that they take two doses of the drug 24 hours before sex and one tablet every day afterwards for the next two days. (This is sometimes called the 2+1+1 method.)
Since the on-demand PrEP project started in 2022, over 700 people have received pills this way from our clinics. Although the shorter course of treatment is easier for people to take, there’s still a chance that they may forget one of the pills, which could lower the protection they’d get from the medicine. For that reason we encourage our 2+1+1 patients to also join an adherence club and the buddy system.
What’s next?
The biggest takeaway from this project is that people are keen to take care of their health; they just need the right information and a supportive environment.
We’re confident that our PrEP project will keep growing. Since we started sharing educational messages on community radio stations such as GugsFM and social media platforms like Facebook in April, we’ve reached more than 100 000 people already, our data reveals.
It’s far more effective, and also economical, to prevent HIV infection than to treat it — studies from around the world confirms it. We should act on that data.