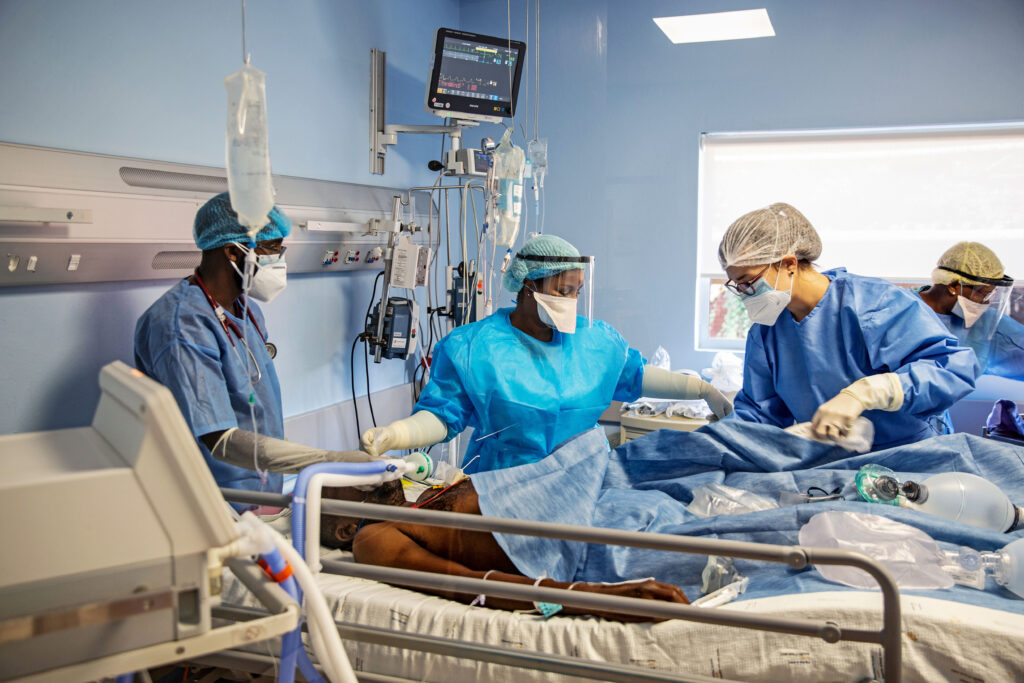
- The Special Investigating Unit has a year to track down dodgy lawyers and patients across the country who file fake medical negligence cases that cost the health department millions in payouts.
- The State Liability Amendment Bill of 2018, plans to decrease how much responsibility the government must take for mistakes that happen at its facilities by limiting the size of medical negligence payouts (for claims over R1-million).
- If the Bill becomes law, victims of medical negligence will be paid in smaller batches instead of one big payout, something actuaries argue could make people too reliant on the government to follow through consistently.
What does it look like when lawyers, patients and state officials collude to cash in on a crumbling health sector?
Fake medical negligence claims for patients who don’t exist (or cases brought for real people with made-up stories), according to Ronel van Zyl, a senior legal advisor for the South African Law Reform Commission (SALRC).
Another scenario involves millions of rands paid by the government for work that state attorneys never did, says Keith Bolton, the former head of paediatrics at the health department’s Rahima Moosa Mother and Child Hospital in Johannesburg.
Bolton is taking a lunch break behind a desk in a colleague’s office.
He’s worked in the public sector for 40 years and has given expert evidence for the state in medical negligence cases for much of that time.
Bolton was also a member of the ministerial advisory committee on medical litigation that developed a strategy to deal with the rise in medical negligence claims at the health department’s 2015 Medico-Legal Summit.
There have been cases, he says, where state attorneys have colluded with “patients” who make baseless malpractice claims, so that they can split the payout. In some instances government lawyers would deliberately not defend the case so that the settlement is bigger.
Bolton says bribes are frequently paid too: Thousands of rands are offered to hospital administrative staff to steal or destroy medical records, because when a negligence case goes to court without the patient’s hospital file, the court regards this as medical negligence in itself.
There’s also something called “touting”, or “ambulance chasing”, which is when lawyers approach potential clients in person.
“I’ve heard stories about agents who single out women with disabled children in the cerebral palsy unit,” Bolton says. “They ask them: ‘How would you like R5-million?’
The tout (someone sent by a lawyer) will physically follow the patient and their file as it goes from one specialist to another. Then, before the administrators pack the file away in a box, the person offers them money for the original file.
Says Bolton: “Six months later, the hospital gets a court summons for a medical negligence case and we have no records.”
What is cerebral palsy and why are medical claims for it so lucrative?
About half of all medical negligence cases in South Africa are for cerebral palsy, a permanent disorder which happens when the developing brain of a foetus or a baby being born is damaged. This results in someone’s muscles being either too rigid or floppy, making it difficult to swallow, to sit independently, walk or talk. Some people may even experience epilepsy and blindness.
There’s little data on how many babies are born with this condition in South Africa, but in 2002, researchers for the South African Medical Journal found 10 in 1 000 children were living with the disorder when they screened about 2 000 children in northern KwaZulu-Natal.
That’s five times higher than the international average overall, which is just over two per 1 000 children, according to a review of 49 studies published in Developmental Medicine and Child Neurology in 2013.
Cerebral palsy cases make for lucrative settlement amounts if there’s a finding of medical negligence because the guilty party (read: in South Africa, mostly the state) often has to pay a settlement amount calculated based on the life-long disability that cerebral palsy causes for someone.
That amount includes the cost of treatments that the person had to get before they went to court. But, according to the Actuarial Society of South Africa (Assa), the aspect that contributes the most to this hefty price tag is all the future costs such as medical treatments, au pair salaries and the home care that someone with cerebral palsy would need. People who win medical negligence claims are also entitled to be paid for the money they would have been able to make, were they not disabled.
On average, claims in South Africa rack up about R5.5-million per case, found a 2021 Assa report.
The SALRC says it’s the sheer size of the awards that draws lawyers to pursue claims against the state.
South Africa’s Contingency Fee Act (or the abuse of it) provides another incentive for attorneys to prowl state hospitals for cerebral palsy cases, the SALRC says, because it allows for something called “no win, no fee”. This means a lawyer’s clients only have to pay for their services if they win the case. But although this Act opens up legal services to people who wouldn’t otherwise be able to afford it, it also opens them up to abuse: lawyers may charge a fee up to a maximum of 25% of the payout. There has been some speculation that some lawyers inflate their fees to 25% even if it doubles their normal fee.
Provincial health departments are littered with corrupt officials
Concocted or fake negligence claims are so common that in July, President Cyril Ramaphosa asked the Special Investigating Unit (SIU) to investigate all nine provinces and the national health department to uncover which government officials, lawyers or other people are defrauding the state.
SIU spokesperson Kaizer Kganyago told Bhekisisa that no further information regarding the corruption allegations can be made public as it is an ongoing investigation, but he said that the report should be completed within a year when it will be sent to the president.
Some experts, however, say such investigations frequently don’t lead to any government action.
Alex van den Heever, an adjunct professor at the University of the Witwatersrand’s school of governance, says the SIU investigation will only be meaningful if its results are made public. “The report must be put in the public domain immediately, not through some political official who can decide what can be disclosed,” he says.
Kganyago says there’s shocking evidence of corruption in medical negligence cases brought against officials working at provincial health departments. “There were previous investigations into maladministration at the office of the State Attorney in 2018 and 2019,” he says. “But the corruption was so bad we had to expand it to the provincial health departments.”
The cost of corruption — and overcrowded hospitals
Valerie Rennie, the head of corporate affairs in the national health department, says these ploys put enormous pressure on the health sector’s coffers.
If none of the claims that are currently on the books for the 2020/2021 financial year are reduced, it will cost the country a combined R120-billion across all nine provinces. Of this, the Eastern Cape would be responsible for close to R39-billion, which amounts to almost a third of the total amount.
The province already had to fork out close to a record-breaking R921-million in this period after the Makhanda High Court shot down the provincial health department’s attempt in June to block people who won their negligence cases from claiming any money. The department argued in court that this amount — about 3.5% of its budget for this period — could topple its already rickety health system and therefore they should be exempted from paying claims.
But corruption is not the only reason for spiralling legal costs, the SALRC’s Van Zyl says.
Reports by the Office of the Public Protector, the South African Human Rights Commission and the Treatment Action Campaign reveal overcrowding, a lack of leadership at health facilities, poor supervision of staff and inadequate management of risks and complaints dating back from 2007.
Says Van Zyl: “Many of the shortcomings identified in 2007 and 2009 have not been addressed to date and are still prevalent.”
SALRC’s 2021 discussion paper warns: “It seems that a number of the provincial departments of health have neither the skills nor the capacity to address the issues highlighted in [such] reports.”
All this is made worse by disorganised and ill-prepared government lawyers. Inertia, lethargy, wasted costs and incompetence are among the allegations that have been levelled at The Office of The State Attorney.
The health department now plans to change the country’s laws to cut the government’s responsibility for medical negligence that happens at its facilities, but some experts say a better goal would be to improve services so that there’s less medical negligence in the first place.
Overburdened staff and negligence go together
Doctors in South Africa’s public sector work under extreme conditions, and they’re often punished for exposing it.
One of Bolton’s colleagues at Rahima Moosa, a paediatrician, Tim De Maayer, was suspended in May (and reinstated a month later) after writing a scathing open letter that detailed, among other things, infections that “spread like wildfire” through the neonatal ward due to poor hygiene, broken equipment, electricity outages and overburdened staff.
Now, back at his desk on the first floor at the hospital, he cautions: “We’ve seen a massive increase in litigation.
“By virtue of being a public service in an adversely constrained environment, there’s going to be negligence happening on a daily basis,” he explains. “Not necessarily the doctor or the nurse but it’s the infrastructure that we work in, the lack of resources and it’s inevitable that things go wrong.”
But the problem with improving the quality of care at hospitals, the national health department’s Rennie argues, is that provincial governments need budgets to do it — and lots of that money is disappearing into medico-legal claims.
“These two problems have to be addressed simultaneously,” she says.
There are, however, already a few plans drawn up specifically to cut down on medical negligence costs by improving both the quality of health care and of state litigation.
For example, the 2016 Medico-Legal Summit Declaration, which was developed by a ministerial task team, sets out ways for hospital staff to brush up patient safety (while they undergo medical treatments) and to reduce the theft of records (for instance, by changing people’s job descriptions to include record-keeping as a responsibility).
In February, the Intergovernmental National Litigation Forum was created in part to improve state legal services. The Forum will help government departments work together to avoid legal costs that result from inefficiency. In a speech Ramaphosa made at the Forum’s inauguration, he explained that government bungles once resulted in a R100-million claim against the state shooting up to nearly R1-billion.
But Van Den Heever argues the state is in denial of its failures. What the health system really needs, he says, is stronger leadership structures that hold the clinical staff accountable for medical negligence and that leave fewer loopholes for collusion.
He concludes: “The department is not actually talking about how they will stop the negligence. They are just trying to make medical negligence cheaper.”
Should medical negligence be cheaper?
The State Liability Amendment Bill of 2018, plans to decrease how much responsibility the government must take for mistakes that happen at its facilities by limiting the size of medical negligence payouts (for claims over R1-million).
One way, the Bill says, is to cap the payments that the government must pay if a victim needs private sector services. The new Bill says the state only has to pay the amount that the same service would have cost at a public facility.
The Bill was rejected by parliament in January last year, because the portfolio committee on justice and correctional services wanted the SALRC to complete an investigation first (which it completed in October 2021). Once the draft legislation is reintroduced as a white paper, the reworked Bill must then be passed by both houses of parliament — the National Assembly and the National Council of Provinces — before it can be signed into law.
The draft legislation also proposes that the health department pay those who win medical negligence cases in a manner other than one lump sum, although the Constitutional Court ruled in 2021 that judges can choose what type of payment(s) the government must make based on the arguments made in court.
If the Bill goes through, it will override the Constitutional Court’s ruling (which gives courts the option to choose what kind of payment works best) and instead make “structured settlements” compulsory for all cases with payouts of more than R1-million. That means that all such medical negligence payouts will be in the form of smaller amounts paid over a period of time.
Another way that the document proposes to make payouts cheaper is by outlawing payments to victims of medical negligence who have passed away.
In 2021, the health department told a justice department portfolio committee that lump sum payments often end up benefiting the estates of claimants, rather than victims themselves, as claimants frequently don’t live long after the court rules in their favour.
As part of an investigation commissioned by the then-minister of justice, Michael Masutha, Van Zyl and her colleagues at the SALRC recommended in their 2021 report that the payments be split into three parts.
One part of the payment is processed immediately, the second bit is paid through periodic payments, and the rest of the amount is paid out as “in kind” contributions, which means the claimant would receive services from a public establishment instead of getting money they could use to go to a private sector doctor.
The SALRC reasons that periodic payments would protect patients from the pitfalls of calculating medical negligence claims, Van Zyl explains. “More than 50% of the money paid out in a lump sum is swallowed by legal fees.”
As a result, many claimants run out of money quickly and then “double dip” by applying for a government grant.
From the national health department’s perspective, this set up would be a more practical and reliable way to make sure people receive the money and services they need, Rennie says.
“Smaller payments might even deter unscrupulous lawyers who are pursuing large payouts.”
But there are drawbacks to the plan, says Assa.
The Society believes smaller payments force people who are entitled to a payout to rely on the government to follow through with the continued deposits. It also doesn’t factor in the unexpected costs that might come up such as costly emergency treatment which large, once-off payments would be able to cover.
Malpractice & collusion — a scourge people won’t talk about
Bhekisisa spoke to 10 medical practitioners who would not go on the record about the collusion, or malpractice they’ve witnessed — even anonymously. They were all worried they would get backlash from the health department, which has strict rules about speaking to the media.
Calling out corruption and poor quality healthcare [in public] is not for the weak, says Bolton. “Not everybody understands it. They say where is your loyalty? This is our hospital, this is our livelihood. Don’t air out dirty laundry in public.”
De Maayer is sitting next to Bolton and listens intently. Even with the door closed of De Maayer’s Rahima Moosa office, the sound of babies crying in the crowded casualty ward bleeds through the walls.
He leans forward in his chair.
“You’re absolutely right, Prof,” De Maayer says. “Our training looks down on someone who calls someone else out for wrongdoing. We protect each other and that needs to change.”
Christina Pitt is a health journalist at Bhekisisa.