- Vasectomy is a permanent contraceptive method. During this surgical procedure, the tubes that take sperm from the testicles to the glands that make semen are cut — in about the time of a lunch break.
- Men’s views on vasectomies are influenced by what friends and family say about the procedure, which often causes untruths about the procedure to spread.
- Many men wonder how much it hurts to get a vasectomy, whether it can be undone later and whether it will ruin their sex life. Three medical experts and a man who has been through it tell it like it is.
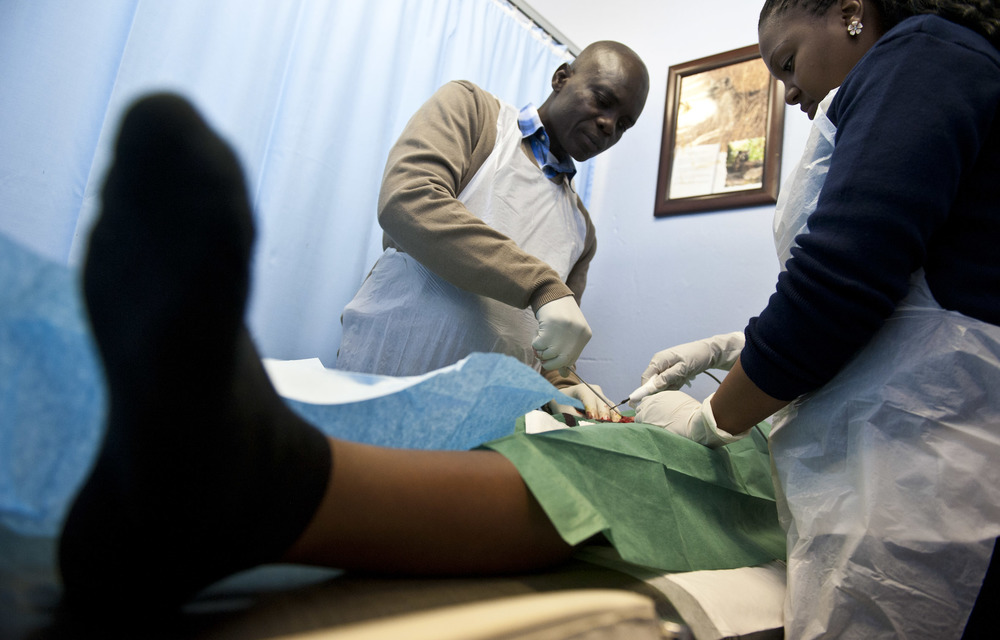
Phetelo Fakude, 29, is staring at the fluorescent ceiling lights of an operating room in a reproductive health clinic in Tshwane. Through the hospital gown he can feel the cold plastic sheet covering the hospital bed — which is not helping much to calm his nerves.
After a few minutes, a nurse and a urologist walk through the doors and come to stand on either side of the bed.
The doctor introduces himself as the one who will be performing Fakude’s vasectomy, a surgical procedure to cut the sperm-carrying tube that runs from each testicle (called the vas deferens) to the glands that make semen and which sit just behind the bladder. Semen is a whitish fluid that keeps sperm cells alive when discharged from the penis when a man has an orgasm.
Fakude turns his head to see the surgeon drawing a clear fluid into a syringe.
“The injection will numb the area around your scrotum,” the doctor explains, which is a good thing, because the scrotum — a pouch of skin that holds the testes — is full of nerve endings and blood vessels, which makes it a sensitive region.
The nurse (let’s call her Sister H) puts a hand on Fakude’s right shoulder and makes small talk. “Where did you grow up?” she asks to distract him from the brief prick of the needle.
By the time she gets to the next question, the anaesthetic must have kicked in because Fakude can no longer feel the doctor’s hand on his groin.
The surgeon nods to Sister H, signalling that they’re ready to start the procedure.
“We’re going to make the main incision now,” the nurse explains. She’s referring to the doctor using a scalpel to make a cut of slightly less than a centimetre along the upper part of the scrotum, just below the penis.
“Breathe,” Fakude tells himself. He doesn’t feel the cut. So far so good, he reckons.
Each vas deferens (there are two, one leading from each testicle) sits on the inside of the scrotum and extends towards the seminal gland, which allows the doctor to lift it up gently with a pair of forceps inserted through the incision.
“We’re going in for the left side first,” says Sister H.
During the prep talk before the procedure, the nurse explained that Fakude might feel discomfort while the doctor is working. This could be because the doctor is pulling the tube somewhat so that he can make the cut.
So he focuses on his breathing to prepare for what’s coming.
The tube is cut and then sealed by passing an electrical current through the tissue briefly. Then the surgeon moves on to the other side and does it all again, before stitching up the cut on the skin. The stitches will dissolve over a couple of days.
The procedure lasts about 10 minutes from start to finish, and then it’s over.
Sister H helps Fakude to put on the Speedo he was told to bring with him (tight-fitting underwear stops the skin from stretching too much, which could tear the stitches open). Then she guides him off the bed and leads him to the recovery room. He lies down and gets an ice pack to place on his groin to limit swelling after the surgery.
You stay in the recovery room for about half an hour so that the nurse can make sure you don’t have any unusual bleeding, Fakude explains.
“You just relax, maybe have a coffee, and then you drive yourself home. It’s the kind of thing you can literally do during a lunch break.”
Things men don’t talk about
After Fakude, who today calls himself a “vasectomy influencer”, tweeted about having had the snip, he realised that men “want to know about these things [vasectomies], but they’re uncomfortable admitting it”.
In a Twitter Spaces event he hosted after his procedure, many men listened, but few joined in the conversation. Yet afterwards many sent him direct messages to find out more.
How can men be encouraged to talk about their reproductive health and family planning?
Hearing from friends or family members can influence a man’s views on vasectomy, a study from Ghana found. “If we even get one person who has done it [vasectomy] to come out and tell us that it is good or he does not suffer from all the problems we have heard concerning vasectomy, I believe it will encourage others to also go and do it,” a respondent said.
But it’s something men don’t talk about easily — because it seems to be wrapped in stigma and misconceptions. “Men do not want to do vasectomy because [they fear] people will make fun of them,” a healthcare worker told researchers in that study.
So, let’s clear up a few things.
Myth 1: It’s going to hurt too much
Often, men’s first question about vasectomies is whether the procedure will be painful, says Sister H. “No procedure is ever painless, not even when you get a tattoo. So, yes, it could be. But it’s less painful than giving birth,” she tells them.
Local anaesthesia is used to prevent the patient from feeling pain during surgery. Numbing creams or medicine to help you relax can also make you feel more comfortable. The doctor could also choose to give you another shot of anaesthetic if necessary. But if it seems just too much to be awake during all of this, you can choose to get fully sedated.
Even though you might feel slight swelling or discomfort for a few days afterwards, you’ll recover fast. Sister H recommends that patients should take it easy for about a week, use pain medication if necessary and try not to exert themselves too much.
In a British study among close to 600 men who had had a vasectomy, only about one in seven reported their scrotum being sore more than six months after the procedure. On average they ranked their pain at about 3.5 out of 10 on a pain measurement scale, where zero means no pain and 10 is the worst pain possible.
A urologist, Smit van Zyl, says complications such as bleeding or infection may occur but are rare, and with a newer technique, where the surgeon doesn’t cut the scrotum using a scalpel but simply pinches open the skin using forceps, the chance of pain, bleeding or infection developing afterwards is small.
Some men may feel a dull ache after having a vasectomy. This usually happens because sperm, which the testicles still make after the procedure, can build up in the part of the tube closest to this gland, says Van Zyl. A simple procedure can be done to relieve the pressure.
Myth 2: It’s easy to undo
No, you have to be pretty sure that you wouldn’t want any children later, because a vasectomy is considered a permanent form of birth control. Sfiso Mazibuko, a urologist from Mpumalanga, explains that although a reversal surgery does exist, it’s a costly, time-consuming procedure that requires highly specialised surgery. The law also requires that you show that you agree to having the procedure by choice.
Men who go for a vasectomy tend to be in their mid-thirties or older and have been in a monogamous relationship for close to 10 years, studies from Ghana, the United States and South Africa show.
Mazibuko says men usually opt for the procedure because they feel their family is complete, and as one patient told him “after six children it was just too much”.
But he cautions that it takes about three months before a man’s semen is sperm free, and couples should therefore use another form of contraception to be safe during that time. You have to go for a semen analysis — a lab test that determines the number of sperm per millilitre of semen — to check if the procedure was successful. “Ideally you want zero sperm in the sample,” says Mazibuko.
Younger men may be more likely to have regrets or change their minds. This is one reason why the health department’s guidelines on contraception stress the need for counselling before the surgery.
Sister H confirms: “They must be 100% sure. They should either not want kids at all or not any more kids.”
Does your sex life change if you’ve had a vasectomy? (It doesn’t)
Myth 3: “You’re no longer a man after having a vasectomy.”
Both Mazibuko and Van Zyl stress that a vasectomy simply prevents sperm being delivered into the semen because the conduit is cut. It’s not the same as castration, which is when the testes are removed. So, you’ll still be able to get an erection and climax, and the amount of ejaculate you pass won’t change because sperm makes up less than 1% of semen.
Also, a vasectomy won’t affect a man’s sex drive, because his testes will still be producing the hormone testosterone, which determines the desire for sex.
A study at Tygerberg Hospital’s family planning unit found that men who had had a vasectomy reported just as good a sex life as men who have not yet had a vasectomy. In fact, sex might even be better after the snip. In a German study that asked heterosexual couples about the quality of their sex life before and after a vasectomy, men said their sexual satisfaction had improved and women said it was just as good as before.
As Sister H tells her patients: “We’re just taking the fish out of the water.”