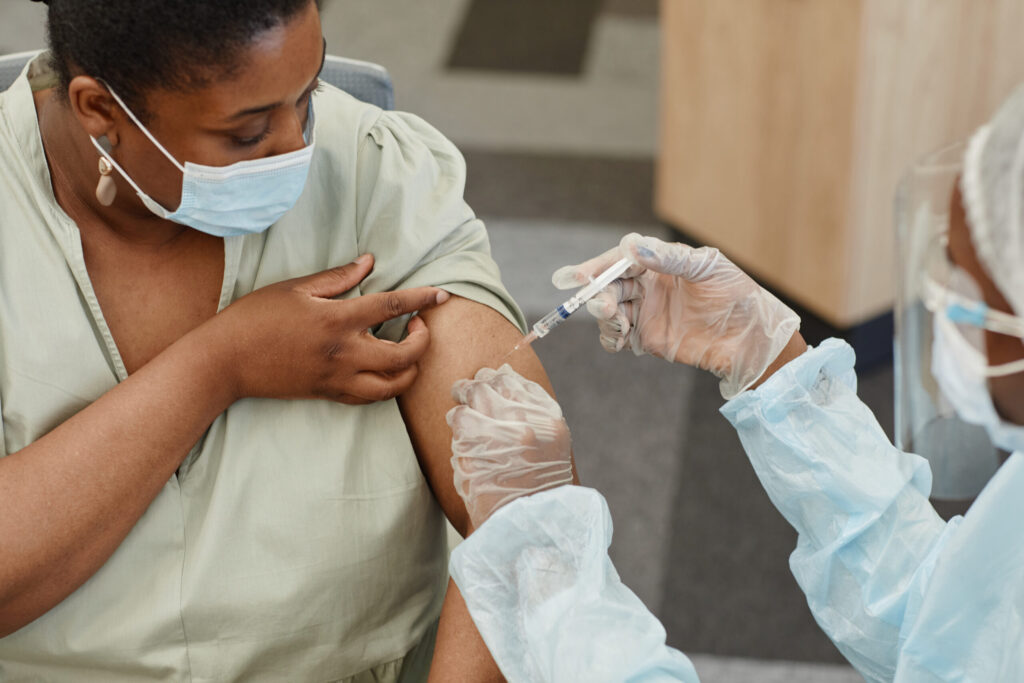
- Up to one in five people can get long COVID — a condition in which someone keeps on feeling ill for months after their initial symptoms have cleared up.
- Paxlovid, an antiviral pill that keeps you from getting very sick with COVID, can lower someone’s chances of getting the long-haul version — but costs around R13 000 for five days’ tablets.
- Ida Jooste, a seasoned health journalist and media trainer, tried to find the medicine in South Africa — with hardly any success. Is it a question of unequal access?
Ida Jooste, 59, was on the hunt for the COVID drug Paxlovid in August.
Paxlovid is a pill that stops the virus that causes COVID from multiplying in your body. Because virus levels (called the viral load) stay low, your immune system can fight the germ effectively. This means you won’t get so sick that you could die or need to go to hospital — with trials showing the chance of dying drops by almost 90% when someone takes the medicine within five days of getting sick.
New research shows it also helps to lower the chance of developing long COVID — a condition in which someone keeps on feeling ill long after the initial infection (called the acute phase) has cleared up, and which can carry on for months, possibly because the virus stays in the body and manages to dodge immune cells.
Symptoms can include anything from chest pain, nausea and bad tummy aches to an incessant ringing in the ears, difficulty breathing, disrupted sleep patterns and an irregular heartbeat — which is why the condition is so difficult to diagnose.
Jooste had been on an almost nine-hour flight from Dubai back home to Durban, sitting across from a maskless man who coughed ceaselessly. Two days after landing, she began to feel like she was getting the flu — except it was very much like when she had COVID in April last year. At the time the illness made her so tired that she couldn’t exercise like before and she struggled to concentrate and remember things — the so-called “brain fog” common in people with COVID.

She didn’t want to go through that again.
Back then, Jooste’s symptoms persisted for long after she was over the worst of the immediate infection — which generally should clear within 14 days — and although she can’t be sure, she wouldn’t be surprised if she had long COVID.
Research suggests that the chance of getting the long-haul version of COVID is linked to how many symptoms someone has when they first get sick, with having more than five in the first week, especially headaches, body aches, shortness of breath and tiredness, upping the chances.
Jooste ticked these boxes. She’s also female and older than 50, two more risk factors for developing the condition.
But the trouble is that long COVID is difficult to pin down because there’s no exact diagnosis — nor do we know definitively how it develops, says Resia Pretorius, head of the department of physiological sciences at Stellenbosch University.
From research by Pretorius and her team, it appears that the condition affects nearly every organ system because the virus damages the lining of blood vessels — everywhere in the body — which affects how things like immune cells, oxygen and nutrients move into and out of the bloodstream.
Because hardly any of the symptoms of long COVID are specific enough to confirm a diagnosis, and because there’s neither a definitive test nor an agreed definition, the illness is often dismissed as being all in one’s head.
“It’s a diagnosis of exclusion, where clinicians must know exactly what they’re looking for,” says Pretorius, “and unfortunately there are very few such clinicians.”
Chasing a unicorn
With an uncertain diagnosis, getting medicines that might help to prevent it is not a priority for most doctors — nor is it sure whether it’s even worth investing in.
For Paxlovid to work, you have to start taking the pills within five days of starting to feel sick.
Jooste realised she had to get it before the end of the week if she wanted any chance of lowering the chance that she’ll develop severe symptoms or long COVID.
But, as the global health media advisor for Internews, an independent international media organisation, part of her quest was fuelled by journalistic curiosity.
Would the pills be available to everyone equally and easily? Or would getting access to treatment be symptomatic of a divided and unequal health system in South Africa?
Turns out getting the pills was just as hard as getting a script for them.
“I was astonished at how difficult it was to get it [Paxlovid] prescribed,” says Jooste.
While trying to get a script, she also tried to find out where the medicine was stocked.
She called retail chemists in Durban, and then hospital pharmacies too. But none had it. One outlet at a hospital in Umhlanga, part of a large private chain, checked at all their branches — finding the medicine in only a single hospital in Johannesburg.
What a lot it costs
The packet of pills was sent down to Durban and picked up on the last day of the window in which starting treatment would be effective.
But is the difficulty in getting hold of the medicine only a question of unequal access?
Despite the South African Health Products Regulatory Authority registering Paxlovid in January, the medicine “is not widely available in South Africa,” says Andy Gray, senior lecturer in pharmacology at the University of KwaZulu-Natal and a member of the National Essential Medicines List committee, who advises the government on what medicines to buy for state facilities.
At just over R13 000 for the five-day course, “it’s priced out of reach of most,” says Gray. “It’s not recommended for the national list of essential medicines.” (This means the health department won’t buy it.)
But price isn’t the only deciding factor; there are many other things that need to be taken into account too when the government has to choose which medicines they buy for the country — determining whether it’s practical and how many people will really benefit come into play too.
[WATCH] Tech talk: Unpacking and assembling the puzzle pieces of a COVID vaccine
“Starting treatment after a diagnosis within a few days of the onset of symptoms is a challenge,” Gray explains. A patient would need to go for a COVID test, and the doctor would have to check whether Paxlovid could be an option for them, as it can interact with many other drugs — all this before the tablets can be dispensed by a pharmacy.
“Not everyone would be able to get a test or seek care early enough for the treatment to work,” he says.
But, he says, an even bigger problem is that it’s hard to know how much having medicines like Paxlovid available would benefit the country, even if South Africa does get a lower-priced version of the pills.
The drug has been approved for generic manufacture through the Medicines Patent Pool, but no pharma companies have applied to register it so far, says Gray. Moreover, a generic form of the medicine would only be sold to the state.
“There’s a theoretical benefit that maybe Paxlovid will do something to long COVID, but we don’t know who’s at risk [of developing the disease]. And we don’t know if there’s strong evidence that changing the viral load early translates into a different [result].”
Being tired of being tired — and not knowing why
The chance for long COVID is higher in women, people over 50 and those with other health problems, for example high blood pressure or diabetes — factors that mean it’s not unlikely that more than the estimated 10–20% of people who had COVID could go on to develop the long version.
Of the people who do get long COVID, one in 10 have to stop working. In a global survey around half of people with long-lasting symptoms could not work a full day six months after they first got sick and about a quarter were not working at all by then because they were exhausted after doing even simple everyday things like washing dishes or walking to the shops and their heads feeling foggy.
The non-descript cluster of symptoms in long COVID look similar to myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS for short) — a condition in which someone gets extremely tired after doing simple physical or thinking tasks and which could develop after becoming infected with a common type of herpes virus (called the Epstein-Barr virus).
Despite symptoms being described in medical texts for almost 90 years already, doctors started to accept it as a real disease only from the mid-1990s, leading to the condition being stigmatised and diminished — much like long COVID.
“People with ME/CFS were simply not believed [in the past], and told their symptoms are all in their minds,” says Pretorius. But just because there isn’t a biomarker or diagnosis for a condition yet, doesn’t mean it doesn’t exist — it simply means we still have to find it — just like it was for ME/CFS in the past.
“We don’t understand all the changes [in our bodies] from COVID, which result in the many different symptoms presenting as long COVID,” says Gray. “And without that, we don’t know how to treat it.”
Research should first try to understand the condition and diagnosis, rather than interventions like Paxlovid, he says.
Did Jooste find the answer she was looking for in her quest for Paxlovid?
She’s not sure: “With or without the drug, with long COVID there’s going to be inequities about access to paid leave, hospitalisation and information.”