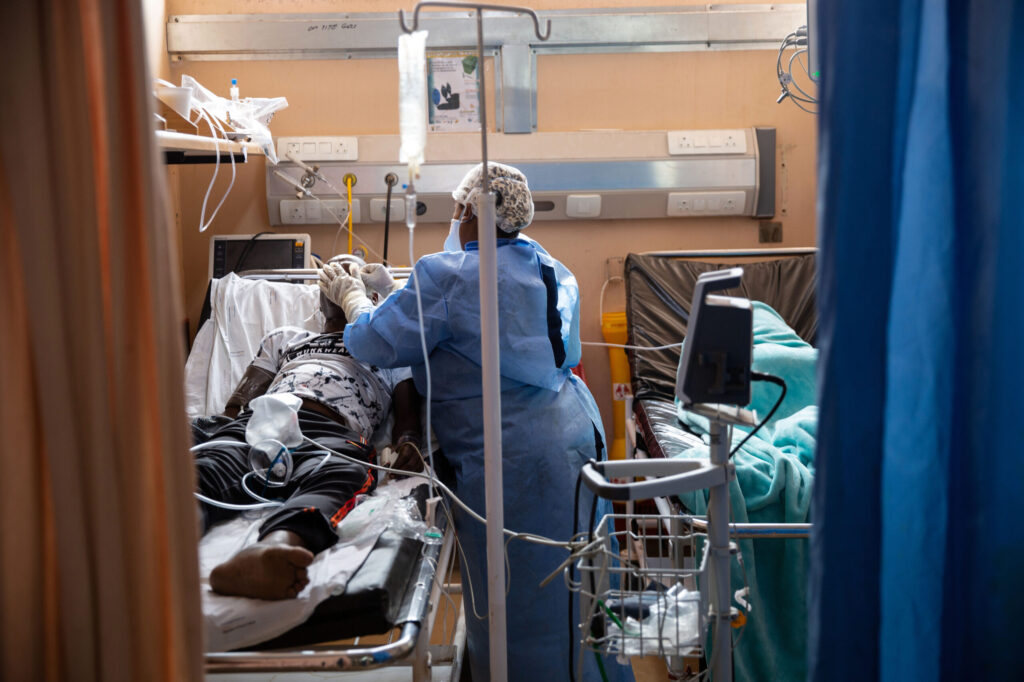
- World leaders are tackling the question of universal health coverage (UHC) — and the dismal progress since 2019 — at today’s high-level meeting at the 78th United Nations General Assembly in New York.
- A political declaration on the table asks delegates to commit to speed up the process for giving everyone access to good-quality health services for free — because we’re not even halfway to the target set at the previous round of talks in 2019.
- South Africa’s version of UHC is the proposed National Health Insurance (NHI) fund, which will be a single, centrally administered pool of funds from which the state will pay for health services for everyone.
- We’ve put together a collection of our previous coverage on the NHI — to help you be part of constructive debate.
Today, on the third day of high-level meetings at the 78th United Nations General Assembly in New York, political leaders are discussing how to speed up people’s access to universal health coverage (UHC) — which means everyone having access to good-quality health services when and where they need it without it having to cost them an arm and a leg.

It’s been on the world’s radar for a decade already, and was formally put on the development agenda in 2015, when member states committed to work towards covering their people’s healthcare needs by 2030.
But a joint report by the World Health Organisation and the World Bank says we’re far off the mark in reaching the targets that were penned at the previous round of high-level discussions, in 2019 — the most notable one being that 523-million people in the world don’t have access to affordable good-quality healthcare yet — half the number that was aimed for in 2019.
South Africa’s version of UHC is the proposed National Health Insurance (NHI) fund, for which the Bill was passed by Parliament’s National Assembly in June. Its aim is to set up a national fund from which health services for all will be paid.
At the moment, South Africa has an unequal, two-tiered health system, where health spend is split about 50-50 between public and private services — yet about 80% of the country’s population depend on using state facilities.
The idea of the NHI fund is getting people hot under the collar, though, because there’s doubt about trusting the government with administering funds in a transparent manner to the benefit of all citizens and fixing a broken public health system — without money being squandered.

If the NHI Bill becomes law, it will mean that private medical schemes will essentially cease to exist, as they will be allowed to cover only services not included in the proposed NHI scheme’s package. But exactly how this will be administered is not clear yet, and for the next three years at least South Africans are unlikely to see much changing in how we pay for healthcare — which for many will mean continued high out-of-pocket healthcare costs or having to accept a frequently dismal public health service. It’s two opposite ends of a spectrum.
On the page we put together here, you can read or watch how we’ve covered questions about the proposed NHI fund before — all in one place — to give you insight into what you can expect from the idea of UHC in South Africa, what you should be concerned about, and why the path to getting there is not a simple one.
[READ] The health department’s NHI branch appointed two new chief directors in July. Here’s what you need to know
Does throwing money at badly managed government clinics and hospitals result in better services? Dave Martin thinks no. He lives in the rural Eastern Cape and has been using public facilities for the past two decades.
[READ] NHI: The problem with trying to kill two birds with one stone — an op-ed by rural development specialist Dave Martin

But, says Nicholas Crisp, the head of the NHI, things are not as black and white as Dave Martin puts them: we can’t wait for public health services to be perfect before we start with UHC; we need to fix these as we go along.
[READ] Right of reply: “It’s far more complex” — the head of the NHI, Nicholas Crisp, responds to Dave Martin’s op-ed

South Africa doesn’t have nearly enough doctors who are prepared to work in rural areas — and even when they are, provincial health departments don’t have the budgets to appoint them. We’re basically training more health workers than the government can afford to appoint. Can the NHI fix this? Well, yes — and no.
[WATCH] Health Beat #4 | Can the NHI fix SA’s rural doctor dilemma?
How do breast cancer services in the private and public service compare? When we investigated this, our team expected a clear “public services are bad” and “private services are good” scenario. But, to our surprise, the answer wasn’t nearly as simple. Watch this Health Beat episode to find out why.
[WATCH] Health Beat #9 | Cancer and the NHI: Will patients see better treatment?
How will the NHI be funded? Taxes and possible salary deductions, based on a proportion of what you earn. Those “deductions” will essentially replace your medical aid premiums, as the NHI Bill (if it’s passed by parliament in its current form) will make it illegal for schemes to pay for services which the NHI already provides — medical aids will only be allowed to pay for “top up” services.