Bhekisisa looks back at, and follows up on, some of the most popular and impactful stories of 2013.
Since the M&G Centre for Health Journalism, Bhekisisa, was established last year, it has covered pressing health issues in both South Africa and abroad.
Some of the stories have had a direct impact on the people involved whereas others were met with disregard by authorities.
Here are the pieces that have aroused the most interest among our readers.
Officials galvanised by isolated haven’s cry

“All hell has broken loose since the publication of your story about our home,” Alex Gunter, the head of Ikhaya Loxolo, a home for the mentally disabled near Elliotdale in the Eastern Cape, told the Mail & Guardian.
On November 8 2013, Bhekisa published a story, “If they are raped, then so what?”, that investigated the rape of mentally disabled girls and adolescents in Hobeni village in the Elliotdale area and the alleged refusal of government social workers to assist parents with mentally disabled children to find homes.
The article also looked into the Eastern Cape department of social development’s alleged refusal to accept funding proposals that Ikhaya had submitted in 2004, 2005, 2006 and 2008.
As a result of the story, Ikhaya has received up to R10 000 in cash donations and several promises of clothes and equipment for their mentally disabled residents.
“But what has excited us most is a high-level meeting with the Eastern Cape social development department in which we have agreed on timelines and goals for the future,” Gunter said. “We have also received very useful assistance from the Eastern Cape health department with registering as an official service provider that will enable us to qualify for more types of government funding.”
The week after the story was published, a team from the Eastern Cape health department was commissioned by Parliament to visit the home.
According to the Eastern Cape social development spokesperson, Gcobani Maswana, who attended the meeting with Ikhaya, social workers complained that they did not have transport to visit Hobeni.
“That has now been rectified …and I have personally seen to a 4×4 being made available so that social workers can have one-on-one meetings with villagers with mentally disabled children to assist them and also [hold] group workshops to encourage them to send their children to Ikhaya and apply their kids’ disability grants effectively,” Maswana said.
He said his department has also put a process in place to assist Ikhaya to apply for social development funding and ensure the applications are accepted for review.
An M&G reader and mother of a disabled child, Pennellope Jonesa, commented online: “How on earth can someone say what we read in the heading [‘If they are raped, then so what?’]?!? My word, it’s shocking and downright inhuman and selfish! Thank goodness for people trying to help these people.”
Broken machines and shortages vex Baragwanath
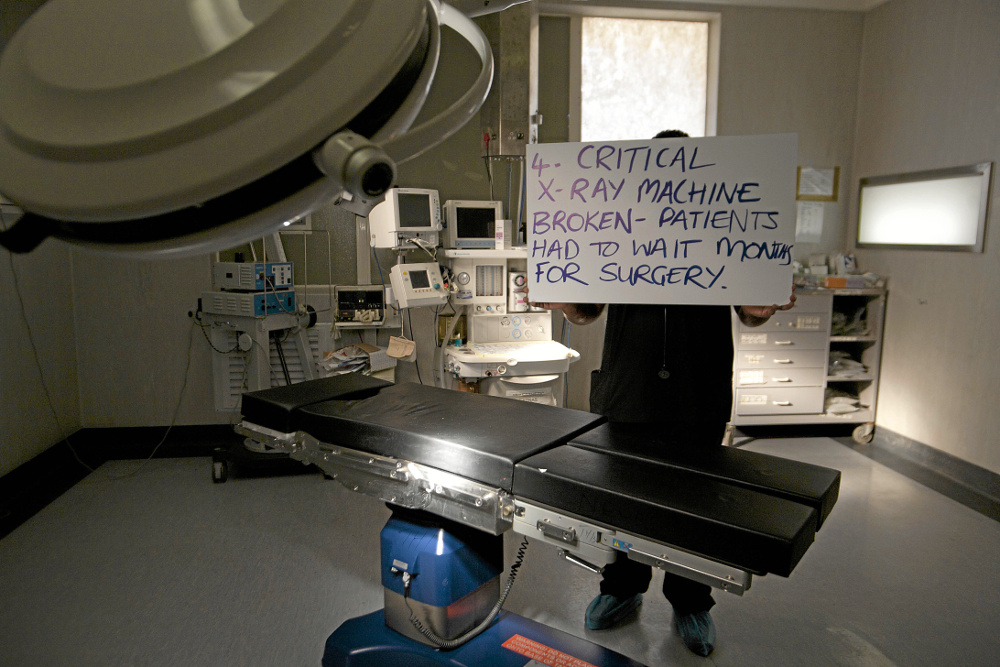
In a “last resort” to improve working conditions and consequently the quality of care they give to patients, eight doctors from Chris Hani Baragwanath Hospital in Soweto approached the Mail & Guardian in October with a list of problems they were experiencing at the facility.
Broken equipment, medication stock-outs and a lack of resources to deal with the enormous patient load were some of their concerns (published on October 25 2013), which were either ignored or treated with a lack of urgency by hospital management.
But their complaints seem to have fallen on deaf ears – hospital management has done almost nothing about their working conditions.
“In the two months since the story was published things have actually worsened,” complained one of the doctors.
One of the biggest issues raised by the doctors, which had dire implications for patients, was that broken equipment took months to get fixed if fixed at all.
A broken x-ray machine resulted in many botched operations in the orthopaedics department that had to be redone.
But, since the publication of the M&G story, the hospital has experienced more equipment break-downs.
“We have two CT scanners [computerised tomography scanners, which take detailed x-ray images of internal structures in the body and can be used to diagnose many conditions] and one broke about a month ago and it still hasn’t been fixed,” another doctor said.
“I spoke to one of the radiologists, who said the reason it hasn’t been fixed is because the previous repair bills haven’t been paid and the company refuses to help until they get their money,” he said.
Gauteng health department spokesperson Simon Zwane said: “I know that hospital management is attending to the issue to get that working but there is still the other one, which is operational.”
But doctors say that, because of the extra load, the only working scanner is also “starting to give problems”.
According to doctors, even urgent cases aren’t being attended to because there are too many patients for one scanner.
“I had a patient who came in yesterday urinating a lot of blood. Today he is still only number 26 on the list and we can’t do anything until we find the cause of the blood – and for that we need to do this scan,” said one doctor.
He said the urgency of this patient’s case means that a scan should have been done immediately after he was admitted.
Another concern raised was that, at Lillian Ngoyi Clinic, right next to the hospital, there was no working electrocardiogram machine, which measures the heart’s activity and can detect a heart attack, an enlarged heart or heart failure, as well as many other conditions.
According to Zwane, the electronic functioning of the machine was in order and that “staff broke the lid during use”.
He said that the hospital had asked for a technician to replace the lid soon.
One M&G Online reader, posting anonymously, commented: “I spent three years at Bara, dealing with the same issues. Basic levels of hygiene and care were completely ignored by a fat, lazy chief executive who sat in her ivory office tower with beautiful furnishings while our poor patients languished in unsanitary conditions. There was even a time when Panado was out of stock at the pharmacy! I couldn’t deal with the working conditions, the inability to serve these poor people who deserved so much more.”
Talks on clear-cut solutions initiated

In September this year, doctors and traditional leaders started negotiations to allow doctors to assist with circumcisions in an effort to reduce the number of initiation-related deaths and injuries in Pondoland.
A Bhekisisa article on the victims of botched traditional circumcisions in the area has played a pivotal role in this development. “The boys who lost their manhood”, published on August 16, resulted in the health organisation TB/HIV Care contacting Dingeman Rijken, a doctor at the Holy Cross Hospital near Flagstaff at the time. He was quoted in the article.
“After reading the story, I googled Dr Rijken’s contact details and got in touch with him,” said Carlos Orte from TB/HIV Care.
“I thought there must be a way to collaborate, as our doctors have been conducting medical male circumcisions in the Eastern Cape for quite some time. We have, however, had serious problems with the uptake of our services, as medical circumcision is often not acceptable from a traditional point of view.”
According to Rijken, the story led to a solid collaboration.
“Because I had strong relationships with traditional leaders and the royal house in Eastern Pondoland, I was able to put TB/HIV Care in touch with them and together we presented a proposal to the royal house on how we could work with them.”
“The terribly messed-up lives of boys described in the article … shocked the leadership into speeding up their efforts to come up with a plan to make circumcisions safer,” he said.
“It has also helped to increase awareness of the issue among provincial and national government leaders and is also partly why Health Minister Aaron Motsoaledi has asked me and Community Development Foundation director Nkululeko Nxesi to write an advisory report for him with suggestions on how to solve this appalling situation.”
However, a week before the December 2013 initiation season, negotiations became “extremely complicated”, with traditional leaders saying they didn’t have enough time to implement the discussed plans and postponing “solutions” until the next initiation season in June.
Maternal deaths highlight poor state of hospitals

The human rights organisation Section27 and HIV advocacy group the Treatment Action Campaign (TAC) on World Aids Day used a story about maternal deaths to illustrate the dire state of Mpumalanga hospitals.
“We are concerned about the lack of quality in healthcare service provision, as highlighted by cases such as a woman who lost her life due to negligence at KwaMhlanga Hospital, as recently reported by the Mail & Guardian,” the TAC and Section27 said in a letter to deputy president Kgalema Motlanthe.
Mpumalanga TAC co-ordinator Thobile Maseko said the Bhekisisa story “was the evidence we needed to present to the deputy president to drive the point of the poor state of KwaMhlanga Hospital and high maternal mortality rates home”.
The story detailed an account by Selena Msiza from Vlaklaagte 2 whose daughter, Lindiwe, had given birth there. Msiza said doctors “performed a Caesarean section, but had no idea she was expecting twins”.
“After taking out the first baby, they started to stitch her up. But my daughter said she told them that she could feel that there was another baby moving inside.
“They had to remove the stitches and open her tummy again. That’s when they saw the second baby and took him out,” Msiza said last year. Lindiwe died a week later.
A senior official in the Mpuma-langa health department, who asked not to be named, said that the story has led to the department investigating maternal health issues at the hospital, as well as the state of the hospital building and equipment, and staff training.
Health professionals smacked on the wrist

Two Western Cape medical specialists have been found guilty of insufficient care and fined R 15 000 each by the Health Professions Council of South Africa (HPCSA), the body that regulates health professionals, for misdiagnosing a patient in April 2011.
The patient, businessperson Jasper Hoon, is not happy with the verdict. “I was told that this is the highest sanction that a doctor can get even if the patient dies of neglect,” he said.
The ruling comes after Bhekisisa published a story on August 2 2013 about Hoon’s criticism that the council was “dragging its feet” in handling grievances from the public against doctors.
His view was shared by a Mail & Guardian reader, “SR”, who left the following comment on our online platform: “In my opinion, the HPCSA is slow and inefficient and gives their members the benefit of the doubt. It is simply not worthwhile complaining to them as they protect their members.”
Hoon filed a complaint against an orthopaedic surgeon and a neurosurgeon who treated him for back pain after he had sought help for “crippling pain” in one of his legs. Months later Hoon was hospitalised and diagnosed with deep vein thrombosis, a condition that occurs when a blood clot forms in one or more veins that are deep in the body, usually in the legs.
The delay in getting the correct treatment as a result of the misdiagnosis meant that Hoon risked losing his foot and has been in a wheelchair for almost two years after undergoing reconstructive surgery.
He says he incurred medical costs of over R1.5-million and lost at least two years of his working life. The development engineer has had to sell one of his businesses and is unable to work.
His civil claim, which was put on hold pending the council’s decision, will now resume.
“My lawyers are busy finalising the details of my claim and then the subpoenas will be finalised,” he said.















